Fact Finder - Science and Nature
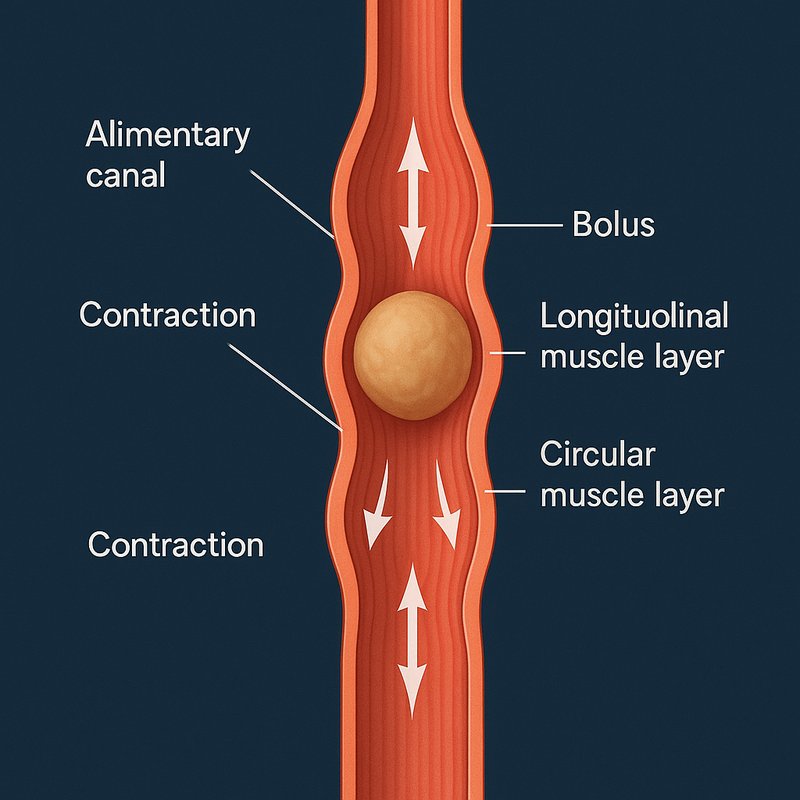
Alimentary Canal: Peristalsis
Peristalsis is the wave-like muscle contractions that push food through your alimentary canal without any conscious effort on your part. Your digestive tract's inner circular and outer longitudinal muscles work together, narrowing behind a bolus while widening ahead of it. Your enteric nervous system controls this process independently, using chemicals like acetylcholine and serotonin to regulate the waves. There's plenty more fascinating detail waiting just ahead.
Key Takeaways
- Peristalsis consists of involuntary wave-like smooth muscle contractions that propel food and fluids through the entire alimentary canal.
- Two coordinated muscle layers work together: the circular layer narrows the lumen while the longitudinal layer widens the passage ahead.
- The small intestine generates approximately 16 peristaltic waves per minute, while the large intestine produces only 2–4 daily.
- Specialized pacemaker cells called interstitial cells of Cajal generate electrical slow waves that trigger rhythmic smooth muscle contractions.
- Peristalsis is controlled by the enteric nervous system independently, using chemicals like acetylcholine to contract and nitric oxide to relax muscles.
What Is Peristalsis and Why Digestion Depends on It?
Keeping food moving through your digestive system depends on a process called peristalsis — wave-like, involuntary muscle contractions that push contents through the alimentary canal. Your longitudinal and circular smooth muscles work in coordination, contracting and relaxing rhythmically to propel food forward. The medulla oblongata controls this process, triggering muscle responses when food or fluids enter your GI tract.
Peristalsis isn't just about movement — it's essential for nutrient timing, ensuring food spends adequate time at each digestive stage for proper breakdown and absorption. It also clears bacteria and waste products before they accumulate. The clinical implications are significant: when peristalsis is disrupted, your entire digestive function suffers. Without it, eating and waste elimination become impossible, making peristalsis one of your body's most critical involuntary functions. When peristalsis moves too fast or too slow, it creates motility disorders that can result in conditions ranging from diarrhea and constipation to bacterial overgrowth and nutritional deficiencies.
The Muscles and Anatomy That Power Peristaltic Movement
Powering every wave of peristalsis is the muscularis propria — a dual-layered muscle structure sandwiched between the submucosa and serosa of your GI tract wall.
It consists of an inner circular layer and an outer longitudinal layer of smooth muscle, each playing a distinct mechanical role.
The inner circular layer narrows the lumen behind a food bolus, pushing it forward.
The outer longitudinal layer shortens the tract ahead of it, widening the passage.
Coordinating these movements is the myenteric plexus, nestled between both layers.
When a bolus distends your intestinal wall, stretch receptors trigger afferent signaling that activates motor neurons within the plexus.
This initiates the alternating contraction and relaxation cycles that generate the synchronized, wave-like motion driving food through your entire digestive tract.
Interstitial cells of Cajal serve as the gut's pacemaker cells, generating and propagating slow waves that depolarize smooth muscle to sustain the rhythmic timing of each peristaltic contraction.How Peristaltic Waves Move Food Through the Digestive Tract
Once food enters your digestive tract, peristalsis drives it forward through a continuous sequence of coordinated muscle contractions and relaxations. Circular muscles behind food contract while muscles ahead relax, creating forward momentum. Age-related changes can weaken these contractions, contributing to swallowing disorders and slower transit.
Key peristaltic wave facts:
- Primary esophageal waves last 8–9 seconds per swallow
- Secondary waves activate when food gets stuck, continuing until it reaches your stomach
- Small intestine waves cycle approximately 16 times per minute
- Large intestine waves occur only 2–4 times daily
- Wave intensity peaks within one hour after eating
This wave-like pattern operates continuously from your esophagus through your rectum, efficiently moving contents forward while supporting digestion and absorption at each stage. The entire process is coordinated by the myenteric plexus, an interconnected neuronal network running from the esophagus to the rectum that governs peristaltic wave activity.
Where in Your Body Each Stage of Peristalsis Occurs
Peristalsis doesn't confine itself to a single location — it's a body-wide process, with each organ playing a distinct role.
It begins in your oral cavity, where chewing forms a bolus before swallowing triggers primary peristaltic waves through your pharynx and esophagus.
Your stomach then churns food into chyme over roughly three hours.
From there, your small intestine's gentler, rhythmic waves handle most nutrient absorption over three to six hours.
Your large intestine compacts waste, absorbing remaining water before peristalsis pushes stool into your rectum for storage. This absorption process causes the remaining waste products to become increasingly more solid over time.
Even beyond digestion, peristalsis works through your ureters, bile ducts, and vas deferens.
Muscles extending to your pelvic floor ultimately coordinate the final elimination of waste, completing the full journey peristalsis facilitates throughout your body.
The Nerves and Chemicals That Control Peristalsis
Behind every rhythmic squeeze of your digestive tract, a sophisticated network of nerves and chemicals calls the shots. Your enteric nervous system drives peristalsis independently, while neurotransmitter modulation fine-tunes each contraction and relaxation cycle.
Key players in enteric reflexes include:
- Acetylcholine and Substance P trigger smooth muscle contraction above the bolus
- Nitric oxide, VIP, and ATP relax muscles below the bolus
- Serotonin (5-HT4 receptors) amplify peristaltic force by boosting acetylcholine release
- Parasympathetic pathways enhance motility through vagus nerve signaling
- Sympathetic pathways suppress gut activity, opposing parasympathetic effects
Your myenteric plexus coordinates these signals by relaying stretch and chemical information through interneurons, triggering synchronized muscle contractions that push food efficiently forward. The myenteric plexus runs continuously from the upper esophagus all the way to the internal anal sphincter, ensuring peristaltic control spans the entire length of the digestive tract.