Fact Finder - Science and Nature
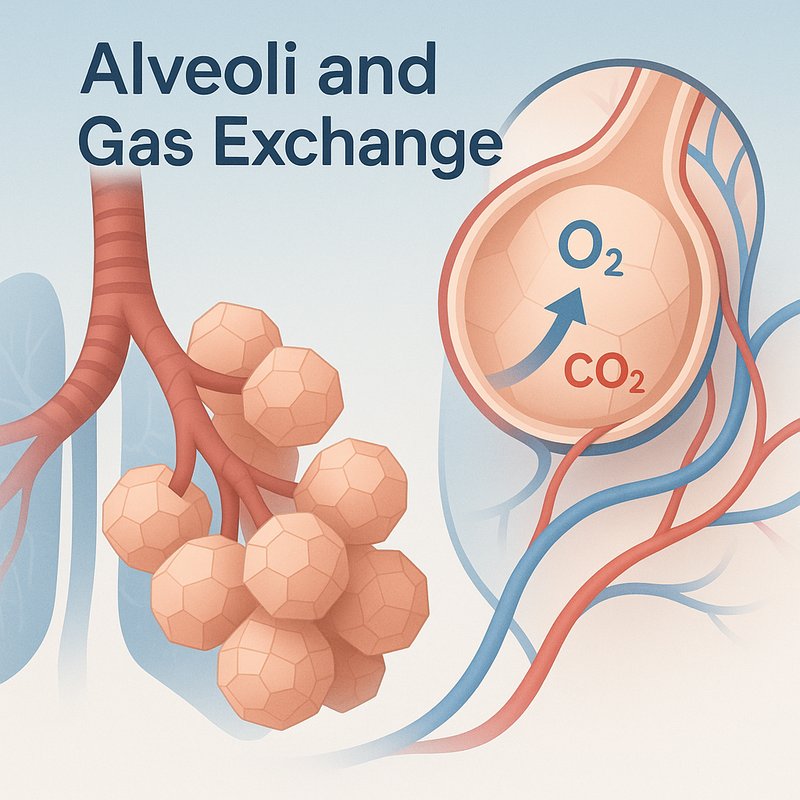
Alveoli and Gas Exchange
Your lungs pack roughly 480 million alveoli into a chest barely the size of a football, creating up to 118 square meters of gas-exchange surface — larger than a racquetball court. These tiny air sacs aren't round bubbles; they're interlocking polyhedra sharing flat walls. Oxygen crosses an air-blood barrier as thin as 200 nanometers, reaching your bloodstream in milliseconds. There's far more to how these microscopic structures keep you alive than most people ever realize.
Key Takeaways
- The lungs contain approximately 480 million alveoli, providing a total gas-exchange surface area of roughly 70–100 square meters.
- The air–blood barrier can be as thin as 200 nanometers, allowing oxygen and carbon dioxide to diffuse rapidly between air and blood.
- Capillaries wrap each alveolus, covering roughly 70% of its surface, maximizing contact between blood and inhaled air.
- Gas exchange is perfusion-limited, with oxygen and carbon dioxide reaching equilibrium just one-third along the capillary length.
- Type II pneumocytes produce surfactant, reducing surface tension and preventing alveolar collapse, especially critical in premature newborns.
What Do Alveoli Do in Your Lungs?
Nestled deep within your lungs, alveoli are tiny, cup-shaped air sacs where oxygen enters your blood and carbon dioxide exits.
Located at the distal ends of the bronchial tree, they're organized in grape-like clusters called alveolar sacs. Each alveolus measures between 200 and 500 micrometers in diameter and sits wrapped in a fine capillary mesh covering roughly 70% of its surface.
Concentration gradients drive the exchange process continuously, repeating 12 to 20 times per minute during normal breathing. Oxygen diffuses across the thin alveolar membrane into your bloodstream and travels to tissues throughout your body, while carbon dioxide moves in the opposite direction.
Alveolar clearance keeps your airways clean, removing foreign particles and pathogens. However, respiratory aging can gradually reduce this efficiency, making healthy alveolar function increasingly important over time.
The average adult lung contains approximately 480 million alveoli, providing an enormous surface area dedicated to sustaining efficient gas exchange throughout your lifetime.
How Many Alveoli Are in the Human Lung?
Your lungs contain hundreds of millions of alveoli — around 480 million across both lungs combined, based on design-based stereologic analysis of adult lung specimens. That means each lung holds roughly 240 million, though individual counts range widely from 274 to 790 million total.
This variation isn't random. Developmental variability during early lung growth directly shapes how many alveoli you ultimately have. Larger lungs simply contain more alveoli, since alveolar count closely tracks total lung volume. Aging effects also matter — alveolar walls can break down over time, reducing both count and functional surface area.
Despite the wide range in number, individual alveolar size stays relatively consistent, averaging 4.2 × 10⁶ cubic micrometers. What varies most is how many you have, not how big each one is. This consistency in size translates to an estimated alveolar density of approximately 170 alveoli per cubic millimeter of lung parenchyma.
How Alveoli Are Actually Shaped: Polygons, Not Balloons
Knowing how many alveoli you have is only part of the picture — what they actually look like might surprise you. Despite decades of textbook illustrations showing balloon-like spheres, alveoli are actually alveolar polyhedra — flat-sided, multi-walled structures resembling foam rather than grapes. Each unit shares walls with neighboring alveoli, creating a deeply interconnected network. Synchrotron imaging confirmed this complexity, revealing pores of Kohn that allow direct airflow between adjacent units.
When you exhale, septal mechanics drive the process — alveolar walls fold along pleated corners rather than deflating uniformly. This polyhedral design isn't just structural trivia; it maximizes gas exchange surface area, reduces material waste through shared walls, and enables collateral ventilation. The actual geometry is far more efficient than any simple balloon model could suggest. A typical pair of human lungs contains roughly 480 million alveoli, generating an extraordinary 50–75 square meters of surface area dedicated entirely to gas exchange.
How Your Lungs Swap Oxygen for Carbon Dioxide
Every breath you take sets off a finely coordinated sequence of three interdependent processes: ventilation, diffusion, and perfusion. Ventilation moves 5–8 liters of air into your lungs each minute, while perfusion delivers deoxygenated blood carrying only 40 mmHg of oxygen to your pulmonary capillaries. That steep pressure gradient — versus 100 mmHg in your alveoli — drives oxygen across the respiratory membrane spontaneously, without energy expenditure.
Ventilation heterogeneity disrupts this balance when airflow distributes unevenly across lung regions, reducing exchange efficiency. Alveolar shunting compounds the problem when blood bypasses ventilated alveoli entirely, returning deoxygenated.
Simultaneously, carbon dioxide — at higher pressure in your capillaries — diffuses outward into alveolar air. Remarkably, equilibrium is reached just one-third of the way through the capillary, making gas exchange perfusion limited. The alveolar-capillary membrane is composed of surfactant, alveolar epithelium, basement membrane, and capillary endothelium, each layer representing a potential barrier that diffusion must overcome according to Fick's law.
The Air-Blood Barrier Where Oxygen Enters the Bloodstream
Between each alveolus and the blood racing through its surrounding capillaries sits one of the body's most elegant structures: the air-blood barrier. It's remarkably thin—sometimes just 200 nm—yet strong enough to withstand normal physiological pressures without failing. You'd find it built from three layers: a squamous alveolar cell, a capillary endothelial cell, and their shared basement membrane reinforced by type IV collagen.
This barrier lets oxygen, carbon dioxide, and carbon monoxide pass freely while staying minimally permeable to water, keeping microvascular compliance tightly regulated. Across roughly 100 m² of surface area, gas exchange happens continuously. When pressure differences exceed about 40 mmHg, barrier remodeling fails catastrophically, allowing fluid into the alveoli and triggering pulmonary edema—a serious and life-threatening complication.
Rupture of the air-blood barrier can result in arterial gas embolism, a dangerous condition in which gas bubbles enter the bloodstream and obstruct circulation.
Type I Pneumocytes: The Paper-Thin Cells That Move Oxygen
Lining roughly 90–95% of the alveolar surface, type I pneumocytes are the squamous epithelial cells responsible for moving oxygen from air into blood. You'll find these cells extraordinarily thin—measuring just 0.1–0.2 micrometers—with long cytoplasmic extensions spanning roughly 2,300 micrometers. That thinness minimizes diffusion distance, making gas exchange remarkably efficient.
Their tight junctions and desmosomes maintain barrier remodeling integrity by preventing fluid from leaking into the alveolar space. During alveolar mechanics, these extensions overlap as the lungs expand and contract, keeping surface coverage consistent throughout each breathing cycle.
Though type I pneumocytes are outnumbered two-to-one by type II cells, they dominate surface coverage. Combined with capillary endothelial cells, they form the blood-air barrier that sustains every breath you take. These cells are also known by the synonyms pneumocyte and pneumononocyte, terms used interchangeably across anatomical and clinical literature.
Type II Pneumocytes and the Surfactant You Can't Live Without
Outnumbering type I cells two-to-one, type II pneumocytes cover only 4–5% of the alveolar surface yet drive one of the lung's most critical functions: surfactant production. These cuboidal cells store surfactant components in lamellar bodies and release them to reduce surface tension at the air-water interface, preventing alveolar collapse with every breath you take. Surfactant turnover keeps this system continuously refreshed, maintaining stable lung mechanics.
Beyond surfactant, type II cells handle alveolar repair after injury, replacing damaged epithelium and restoring normal function. Surfactant synthesis begins around week 28 of gestation, which is why premature infants often develop respiratory distress syndrome. Cortisol and thyroxine accelerate production, while insulin suppresses it, explaining the increased risk seen in diabetic pregnancies. Type II pneumocytes have also been proposed to play a direct role in the pathogenesis of COPD, where alterations in their function contribute to surfactant abnormalities and increased airway resistance.
How Alveoli Drive Ventilation, Diffusion, and Perfusion
Alveoli don't just sit at the end of your airways — they actively orchestrate three interdependent processes that keep every cell in your body alive: ventilation, diffusion, and perfusion.
Alveolar mechanics govern how air moves in and out. Negative intrapulmonary pressure pulls air inward during inspiration, while rising pressure pushes it out during expiration. Your alveolar ventilation depends on tidal volume minus dead space, multiplied by respiratory rate.
Diffusion follows pressure gradients — oxygen crosses the thin, moist alveolar membrane into capillaries while carbon dioxide exits. That single-cell-thick lining keeps the pathway short and efficient.
Perfusion completes the cycle. Capillaries wrap each alveolus, though blood flow favors lung bases over apices. When ventilation and perfusion balance at a V:Q ratio of 1.0, gas exchange reaches its peak efficiency.
Why Alveolar Surface Area Is Bigger Than You Think
Most people picture the lungs as two fist-sized sacs — compact, bounded, unremarkable. That image doesn't hold up.
Your lungs pack between 70 and 80 square meters of alveolar surface area inside your chest — exceeding the size of a tennis court. Alveolar folding creates this geometry, layering exchange surfaces into a space you'd never expect.
Each cubic millimeter of lung tissue holds roughly 170 alveoli, and capillaries cover about 70% of each one through microvascular remodeling that maximizes blood-air contact.
Type I epithelial cells line over 95% of that surface, keeping the diffusion barrier thin. Oxygen's low solubility demands exactly this scale. Without it, your blood couldn't absorb enough oxygen to keep you alive.
CT-based quantification research has estimated the total lung surface area in healthy humans at approximately 118 square meters, a figure derived by combining computed tomography analysis with stereologically based histologic measurement.