Fact Finder - Science and Nature
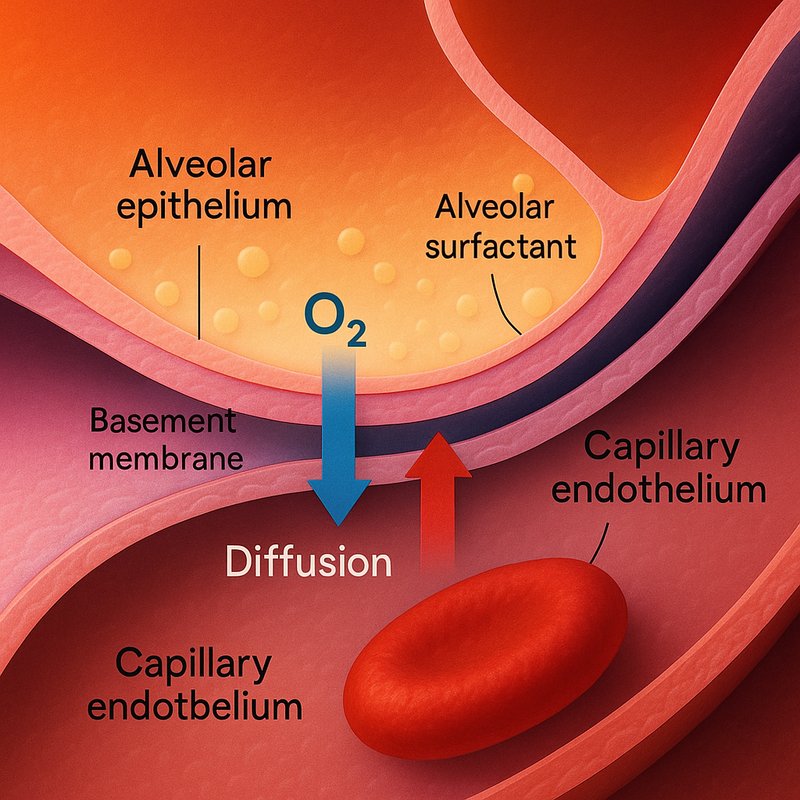
Blood-Air Barrier
The blood-air barrier is one of your body's most remarkable structures. It's thinner than a soap bubble — just 0.57 micrometers in some mammals — yet it handles every breath you take without tearing. It's where oxygen silently crosses into your blood while carbon dioxide exits, all through passive diffusion. A tough collagen band keeps it from rupturing under pressure. Stick around, because there's much more to uncover about this extraordinary tissue.
Key Takeaways
- The blood-air barrier is extraordinarily thin, measuring as little as 0.266 µm in chickens, yet remains strong enough to withstand significant pressure.
- Despite its thinness, the barrier covers roughly 100 m² of surface area in human lungs, optimizing gas exchange efficiency.
- Type IV collagen provides the barrier's tensile strength, maintaining structural integrity even when surrounding cells are damaged or disrupted.
- The barrier is 10,000 times less permeable to water than oxygen, preventing fluid accumulation while allowing efficient gas diffusion.
- Barrier failure can be fatal; its disruption was implicated in millions of COVID-19 deaths as fluid flooded oxygen-exchanging alveoli.
What Is the Blood-Air Barrier?
The blood-air barrier is a thin layer of tissue in the lungs that sits between your capillary blood and alveolar air, forming the critical interface where oxygen and carbon dioxide exchange occurs. You'll also hear it called the alveolar-capillary barrier or membrane. It positions itself between your alveoli and surrounding capillaries, creating the pathway through which gases must diffuse during respiration.
The barrier allows molecular oxygen and carbon dioxide to dissolve on its moist surface before crossing over. Alveolar surfactant supports this process by reducing surface tension and keeping the exchange surface stable. When the barrier sustains damage, barrier remodeling occurs as the tissue attempts repair. Without a functioning barrier, you'd experience life-threatening complications like pulmonary edema or dangerous air bubbles entering your bloodstream.
The barrier derives its remarkable strength from type IV collagen situated between the endothelial and epithelial cells, allowing it to maintain structural integrity despite being extraordinarily thin.
How Thin Is the Blood-Air Barrier?
Measuring just micrometers thick, the blood-air barrier ranks among the thinnest biological structures in the vertebrate body. In rats, the harmonic mean thickness reaches just 0.57 µm, the measurement most relevant to gas diffusion. Chickens, however, outperform mammals dramatically, maintaining a total barrier of only 0.266 µm, with their interstitium measuring a remarkable 0.045 µm.
Comparative physiology reveals striking microstructure variation across species. The crested newt carries the thickest barrier at 2.81 µm, while the mouse holds the thinnest mammalian barrier at 1.27 µm. Chickens display exceptionally uniform layer thickness, unlike mammals, whose higher arithmetic-to-harmonic mean ratios indicate greater structural heterogeneity. Despite its extreme thinness, the barrier maintains low water permeability, preventing fluid accumulation while sustaining efficient gas exchange across roughly 2000 cm² of surface area.
How the Blood-Air Barrier Controls Gas Exchange
Functioning as a precisely engineered selective membrane, the blood-air barrier controls gas exchange through passive diffusion—no energy expenditure required. Gas molecules simply follow concentration gradients: oxygen moves from alveoli into blood while carbon dioxide travels the opposite direction simultaneously.
Your barrier's efficiency depends on two critical factors tied to Fick's equation—surface area and thickness. With roughly 2,000 cm² of alveolar surface area, alveolar ventilation continuously refreshes gas concentrations, maintaining favorable diffusion gradients. Meanwhile, the barrier's sub-micron thickness prevents diffusion limitation, ensuring gases transfer rapidly enough to meet metabolic demands.
Selective permeability completes this system—lipid membranes allow oxygen and carbon dioxide passage while restricting water movement at rates approximately 10,000-fold lower than oxygen diffusion, protecting lung tissue from fluid accumulation that would compromise exchange efficiency. The barrier's thin portion surface area in the human lung spans an estimated 100 square meters, representing roughly half of the total air-blood barrier surface dedicated to optimized gas diffusion.
Why Doesn't the Blood-Air Barrier Just Tear Apart?
Despite being thinner than a human hair, your blood-air barrier withstands remarkable mechanical forces without tearing apart. Its secret lies in sophisticated collagen architecture at its core. Type IV collagen forms an ultra-thin yet incredibly strong band running through the extracellular matrix, providing tensile strength that your cellular layers alone couldn't achieve.
Your body's pressure management strategy adds another layer of protection. Pulmonary capillaries maintain markedly lower pressures than systemic circulation, reducing the hoop stress acting on barrier walls. This evolutionary design keeps pressure differences well below the 40-millimeter-of-mercury threshold where damage occurs.
When extreme pressure does disrupt epithelial and endothelial cells, the extracellular matrix stays intact, acting as your last line of defense against catastrophic barrier failure. When this defense is overwhelmed and fluid begins crossing into the interstitium, lymphatic clearance pathways work to drain excess fluid before it reaches and floods the alveolar air spaces.
What Happens When the Blood-Air Barrier Breaks Down?
When the blood-air barrier breaks down, your lungs begin drowning in their own fluids. Proteoglycan fragmentation dismantles the structural integrity that normally keeps fluid in check, triggering uncontrolled capillary leakage into your air spaces. Gas exchange collapses, and oxygen can't reach your bloodstream.
Here's what barrier failure actually causes:
- Fluid flooding – Blood and serum fill your alveoli, blocking normal breathing
- Escalating permeability – Water and solutes pour through membranes that were once nearly impermeable
- Dangerous cascades – Reactive oxygen species, inflammation, and cell death accelerate tissue destruction
This isn't a rare edge case. Barrier failure drove 7 million COVID-19 deaths worldwide, proving that when this thin membrane fails, the consequences are rapidly fatal. When SARS-CoV-2 disrupts this barrier, plasma floods the alveolar sacs, triggering infiltration of monocytes and neutrophils that amplify lung damage far beyond the initial viral injury.