Fact Finder - Science and Nature
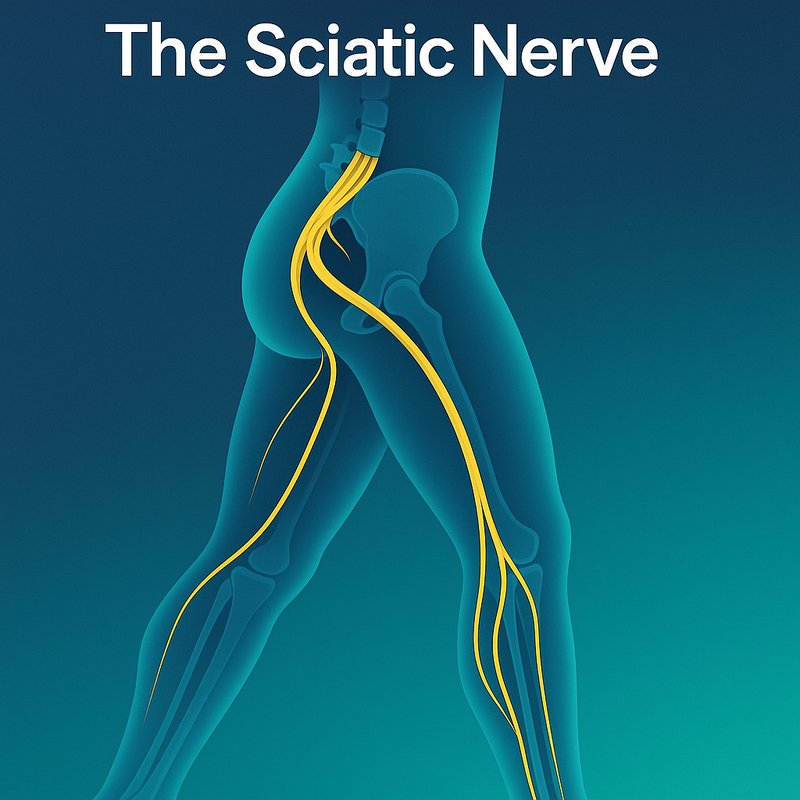
Body's Largest Nerve: The Sciatic Nerve
You probably don't realize that the sciatic nerve running down your leg is roughly as wide as your thumb and longer than any other nerve in your body. It forms from five spinal roots in your lower back, travels through your pelvis, and branches all the way down to your foot. It controls nearly everything below your waist — movement, sensation, and balance. There's a lot more to this remarkable nerve than most people ever discover.
Key Takeaways
- The sciatic nerve is the body's largest nerve, roughly as wide as an adult thumb at its thickest point.
- It originates from five spinal roots (L4, L5, S1, S2, S3) that converge in the posterior pelvis.
- The sciatic nerve actually bundles two separate nerves — the tibial and common peroneal — within one connective tissue sheath.
- It splits near the popliteal fossa into two branches that collectively control movement and sensation across the entire lower leg and foot.
- In approximately 11–16% of people, anatomical variations in its path or relationship to the piriformis muscle exist.
Why the Sciatic Nerve Is the Largest Nerve in Your Body
The sciatic nerve earns its title as the body's largest nerve through sheer physical scale — it's roughly as wide as an adult thumb at its thickest point, dwarfing every other peripheral nerve in the body.
That nerve thickness isn't accidental. It bundles two major nerves — the tibial and common peroneal — within a single connective tissue sheath, creating one powerful structure rather than two separate ones.
Its size also reflects evolutionary significance. Your lower extremities handle complex, high-demand tasks like walking, running, and balancing, requiring massive volumes of motor and sensory information.
The nerve originates from spinal roots L4 through S3, spanning your entire lower body from your lower back to your heel, and its diameter accommodates the sheer fiber load that distance demands. Its long path also exposes it to injury at multiple points, making it vulnerable to conditions like herniated discs and piriformis constriction.
How the Sciatic Nerve Forms and Where It Starts
Forming deep within your lower spine, the sciatic nerve pulls together five separate nerve roots — L4, L5, S1, S2, and S3 — from both the lower lumbar and upper sacral regions. This sacral convergence happens anterior to the piriformis muscle, deep inside your pelvic cavity.
At its pelvic origin, the nerve starts as a flattened band, roughly 5 millimeters tall and 10 to 15 millimeters wide. As these ventral rami unite, they create one thick, combined structure.
The anterior branches of all five roots merge in your posterior pelvis, shifting from individual fibers into a single, large nerve. This mixed nerve carries both motor and sensory fibers, setting the foundation for everything the sciatic nerve controls as it travels distally. Once formed, the nerve exits the pelvis through the greater sciatic foramen, passing inferior to the piriformis muscle as it enters the gluteal region.
Where the Sciatic Nerve Travels From Hip to Knee
After forming in your pelvis, the sciatic nerve exits through the greater sciatic foramen and emerges below the piriformis muscle into the gluteal region. During its gluteal passage, it doesn't innervate any gluteal structures before entering your thigh between the ischial tuberosity and greater trochanter.
As it descends through your posterior thigh, the nerve:
- Runs deep to the biceps femoris long head
- Sits superficial to adductor magnus and short head biceps femoris
- Lies lateral to semitendinosus and semimembranosus
- Stays protected within a continuous fatty sheath from pelvis to knee
- Directly innervates biceps femoris, semimembranosus, semitendinosus, and the hamstring portion of adductor magnus
At popliteal division, the nerve splits into your tibial and common fibular nerves, though 12% of people experience this split earlier at the pelvis. The sciatic nerve also travels alongside the posterior femoral cutaneous nerve as it exits the greater sciatic foramen, sharing the same passage through this bony opening.
What the Sciatic Nerve Actually Controls in Your Leg and Foot
Branching into the tibial and common fibular nerves at your knee, the sciatic nerve controls virtually every movement and sensation below your hip.
Its muscle coordination responsibilities are extensive — the tibial branch manages your calf muscles for plantar flexion, while the common fibular branch drives dorsiflexion and foot eversion through your anterior and lateral leg muscles.
Both branches reach your intrinsic foot muscles, controlling precise toe movements.
The sciatic nerve's sensory mapping covers your entire lower extremity, delivering touch, pain, and temperature signals from your posterior thigh, outer lower leg, heel, and the sole and top of your foot.
Even your adductor magnus receives motor input from the sciatic nerve before it splits, demonstrating how exhaustively it governs lower limb function. Notably, the sciatic nerve is the largest nerve in the human body, reaching roughly the size of a penny at its widest point.
Where the Sciatic Nerve Splits and What Each Branch Does
Near the back of your knee, within a diamond-shaped hollow called the popliteal fossa, the sciatic nerve splits into its two terminal branches — the tibial nerve and the common fibular nerve.
Each branch handles distinct motor and sensory roles, including cutaneous distribution across the lower leg and foot. Nerve compression at this split point can disrupt both branches simultaneously. The tibial nerve further divides in the foot into the medial and lateral plantar nerves.
Here's what each branch controls:
- Tibial nerve travels through the posterior leg to the foot's plantar surface
- Tibial nerve innervates calf muscles, including the gastrocnemius and soleus
- Common fibular nerve wraps around the fibular head laterally
- Common fibular nerve divides into superficial and deep branches
- Deep fibular branch supplies the anterior compartment and foot's medial aspect
How the Sciatic Nerve Varies Between Individuals
Unlike many anatomical structures that follow a predictable template, the sciatic nerve varies considerably from person to person — in how it exits the pelvis, where it divides, and how it relates to surrounding muscles like the piriformis. These anatomic variants aren't rare curiosities; they affect roughly 12% of people and carry real surgical implications.
In most individuals, your sciatic nerve passes inferior to the piriformis intact. But in about 11% of people, the piriformis splits into two sections, allowing part of the nerve to pass between them. The nerve can also divide earlier than expected — sometimes before even leaving the pelvis. Surgeons must account for these variations to avoid nerve injury during procedures involving the hip, gluteal region, or posterior thigh.
In the typical case, approximately 85% of people share the same standard relationship between the sciatic nerve and piriformis, making this the most common anatomical presentation seen in clinical and surgical practice.
Why Sciatic Nerve Anatomy Matters for Pain and Injury
The sheer scale of the sciatic nerve — the largest in your body at roughly 2 centimeters wide — means that when something goes wrong, it rarely goes wrong in a small way. Its course through your body creates multiple nerve entrapment risks, and injuries produce cascading effects across your entire lower limb. Effective rehab strategies depend on pinpointing exactly where damage occurs.
Key anatomical factors driving injury complexity include:
- Compression beneath the piriformis muscle
- Fixed bottleneck through the greater sciatic foramen
- Vulnerability to hamstring injury along the posterior thigh
- Dual tibial and common fibular pathways affected by single lesions
- Proximal injuries producing widespread limb symptoms versus localized distal effects
Around 16% of the population may have anatomical variations in how the sciatic nerve divides or exits the pelvis, which can increase the risk of impingement, entrapment, or irritation.