Fact Finder - Science and Nature
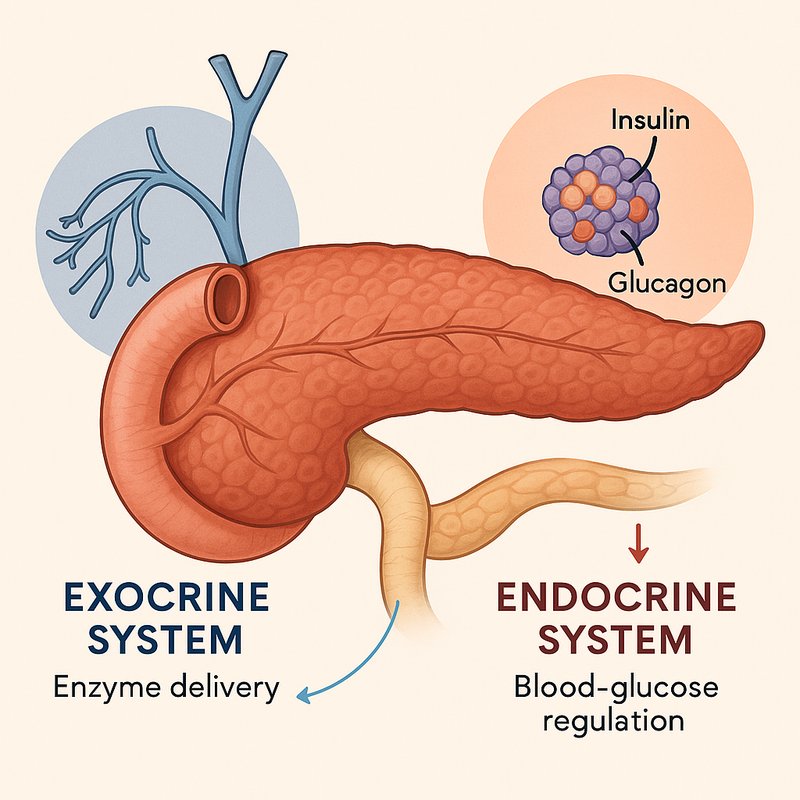
Dual Role of the Pancreas
Your pancreas quietly runs two completely separate systems at the same time — one breaking down your food, the other controlling your blood sugar. It produces up to four liters of digestive juice daily while simultaneously managing blood glucose through insulin and glucagon. These systems share the same organ but operate independently, each with distinct cells, functions, and consequences when they fail. There's far more to this organ than most people realize.
Key Takeaways
- The pancreas runs two independent systems simultaneously: an exocrine system for digestion and an endocrine system for blood-glucose regulation.
- Despite comprising only 1–2% of pancreatic volume, the hormone-producing islets of Langerhans receive 10–15% of the organ's total blood flow.
- The pancreas produces up to 4 liters of enzyme-rich juice daily, neutralizing stomach acid and breaking down fats, proteins, and carbohydrates.
- Insulin and glucagon act as opposing automatic signals, maintaining blood glucose within a precise range of 4–6 mM continuously.
- When both systems fail simultaneously, as in type 3c diabetes, patients experience diabetic symptoms alongside severe digestive failure and nutritional deficiencies.
Why the Pancreas Has Two Completely Different Jobs
The pancreas quietly runs two completely different operations at once, and what makes this possible is its internal organization. Despite sharing a common embryonic origin, its tissues have diverged into two structurally separate systems through tissue compartmentalization.
Acinar cells handle the exocrine side, producing digestive enzymes that travel to your small intestine. Meanwhile, pancreatic islets manage the endocrine side, releasing insulin and glucagon directly into your bloodstream to regulate blood glucose.
Beta cells make up roughly 75% of each islet and produce insulin exclusively. Alpha cells account for about 20% and secrete only glucagon. Because these compartments operate independently, your pancreas can simultaneously digest a meal and regulate your blood sugar without either function interfering with the other. Together, these two systems produce about 1 to 4 liters of enzyme-rich juice daily while continuously adjusting hormone output in response to what you eat.
How the Exocrine Pancreas Powers Your Digestive System
Every day, your pancreas quietly produces around 2,500 milliliters of digestive fluid — a carefully engineered mix of enzymes and bicarbonate that breaks down food and protects your small intestine from acid damage.
Its ductal architecture routes secretions through herringbone-patterned ducts into a 3-millimeter main duct before reaching your duodenum. Pancreatic juices and bile are delivered together into the duodenum, as the main pancreatic duct joins the common bile duct at the ampulla of Vater.
Meanwhile, bicarbonate mechanics raise fluid pH to 8.0, neutralizing stomach acid and activating digestive enzymes.
Three key functions drive this system:
- Enzyme delivery — amylase, lipase, and proteases break down carbohydrates, fats, and proteins
- Acid neutralization — bicarbonate protects your duodenal lining from erosion
- Controlled activation — enzymes only activate upon entering the duodenum, preventing dangerous self-digestion
Your pancreas coordinates all three seamlessly, every time you eat.
The Enzymes Your Pancreas Makes to Break Down Food
Your pancreas produces three primary digestive enzymes — lipase, protease, and amylase — each targeting a specific macronutrient to break it down into forms your body can absorb and use.
Lipase secretion works alongside bile to break down fats, enabling your body to absorb fat-soluble vitamins. Without it, you'd experience diarrhea and fatty stools.
Protease breaks proteins into amino acids while also eliminating harmful intestinal parasites, reducing your infection risk.
Pancreatic amylase converts complex carbohydrates and starches into simple sugars your body uses for energy. A deficiency leaves undigested starch in your colon, causing diarrhea.
Your pancreatic acinar cells synthesize these enzymes at a remarkable rate, storing them in zymogen granules before releasing roughly eight cups of pancreatic juice daily into your duodenum. These enzymes are first translated on the rough endoplasmic reticulum, where newly synthesized proteins undergo critical modifications including glycosylation, disulfide bond formation, and folding into their functional shapes.
Why Pancreatic Enzymes Don't Activate Until the Duodenum
Although your pancreas produces powerful digestive enzymes, it releases them in an inactive form called zymogens to safeguard itself from self-digestion. These protective zymogens only activate when they reach your duodenum, where specific intestinal triggers initiate the process:
- Enteropeptidase, located in your intestinal brush border, cleaves trypsinogen into active trypsin
- Active trypsin then converts chymotrypsinogen, procarboxypeptidase, and proelastase into their functional forms
- The cascade effect guarantees enzymatic activity occurs precisely where digestion is needed
This sequential activation prevents premature enzyme activity that could damage your pancreatic tissue. Premature activation within the pancreatic ducts triggers inflammation and pancreatitis, making this carefully controlled system essential for your digestive health. In pancreatitis, these prematurely activated enzymes attack the pancreas itself, causing the severe abdominal pain that makes this condition particularly debilitating.
The Islets of Langerhans: The Pancreas's Hormonal Control Center
While your pancreas masterfully manages digestion through its exocrine functions, it's equally remarkable as a hormonal powerhouse. German anatomist Paul Langerhans discovered approximately one million microscopic islets distributed throughout your pancreas in 1869. Despite comprising only 1–2% of total pancreatic volume, these structures receive 10–15% of your pancreas's blood flow.
The islet microarchitecture houses five distinct cell types working through precise cell communication. Beta cells (70–75%) produce insulin, alpha cells (20%) secrete glucagon, and delta cells release somatostatin. These cells operate antagonistically — elevated glucose triggers insulin release while suppressing glucagon, and vice versa.
This coordination matters clinically. Beta cell dysfunction causes 100% of type 1 diabetes cases and contributes to roughly 50% of type 2 diabetes cases, making these tiny structures critically important to your metabolic health. Beyond diabetes, islet cell dysfunction can give rise to pancreatic neuroendocrine tumors, which account for approximately 7% of all pancreatic masses and are often slow-growing and well-differentiated.
What Somatostatin, Ghrelin, and Pancreatic Polypeptide Actually Do
Beyond insulin and glucagon, three additional hormones fine-tune your pancreas's regulatory work. Each one targets a specific function, keeping your digestive and metabolic systems balanced.
- Somatostatin signaling slows digestion by suppressing both insulin and glucagon release, preventing hormonal overactivity after meals.
- Ghrelin appetite regulation originates partly in the pancreas, stimulating hunger and prompting you to eat when energy reserves drop.
- Pancreatic polypeptide acts as your body's natural brake after eating — it inhibits exocrine pancreatic secretion, slows gastric emptying, and induces satiety through hypothalamic neuropeptide Y4 receptors.
Together, these hormones don't just react to what you eat — they actively coordinate how much you eat, how fast you digest it, and how efficiently your pancreas responds. Pancreatic polypeptide is synthesized and released by PP cells located predominantly in the head of the pancreas, making that region especially important for hormonal regulation of digestion.
How the Pancreas Uses Insulin and Glucagon to Control Blood Sugar
Somatostatin, ghrelin, and pancreatic polypeptide fine-tune your metabolic responses, but insulin and glucagon do the heavy lifting when it comes to blood sugar control.
When you eat, rising blood glucose triggers your beta response — beta cells release insulin, which moves glucose into muscle and adipose tissues while promoting hepatic glycogen storage.
Once your levels drop four to six hours after eating, glucagon feedback activates alpha cells to release glucagon, breaking down stored glycogen and driving gluconeogenesis in your liver and kidneys.
High glucose suppresses glucagon; low glucose suppresses insulin. These opposing signals operate automatically, keeping your blood glucose between 4 and 6 mM.
Your pancreas effectively runs a continuous, self-correcting loop that responds directly to whatever your bloodstream needs at any given moment. When this loop breaks down, imbalance can lead to conditions like diabetes, which may require prescription hormones to restore proper regulation.
How Pancreatic Dysfunction Leads to Diabetes and Digestive Failure
When your pancreas sustains enough damage to cripple its insulin-producing capacity, the result is type 3c diabetes — a condition that strikes both your endocrine and exocrine systems simultaneously.
Unlike beta cell autoimmunity seen in type 1, this damage stems from physical destruction, including pancreatic fibrosis from chronic pancreatitis or surgical removal.
You'll likely experience symptoms from two fronts:
- Diabetic symptoms — excessive thirst, fatigue, and frequent urination
- Digestive failure — bloating, abdominal pain, and floating, foul-smelling stools
- Nutritional deficiencies — malabsorption of fat-soluble vitamins A, D, E, and K
Managing this condition requires both insulin therapy and pancreatic enzyme supplementation.
Because counter-regulatory hormones are also lost, your blood sugar becomes especially brittle and difficult to control.
Chronic pancreatitis is the leading underlying cause of type 3c diabetes, responsible for approximately 79% of all diagnosed cases.