Fact Finder - Science and Nature
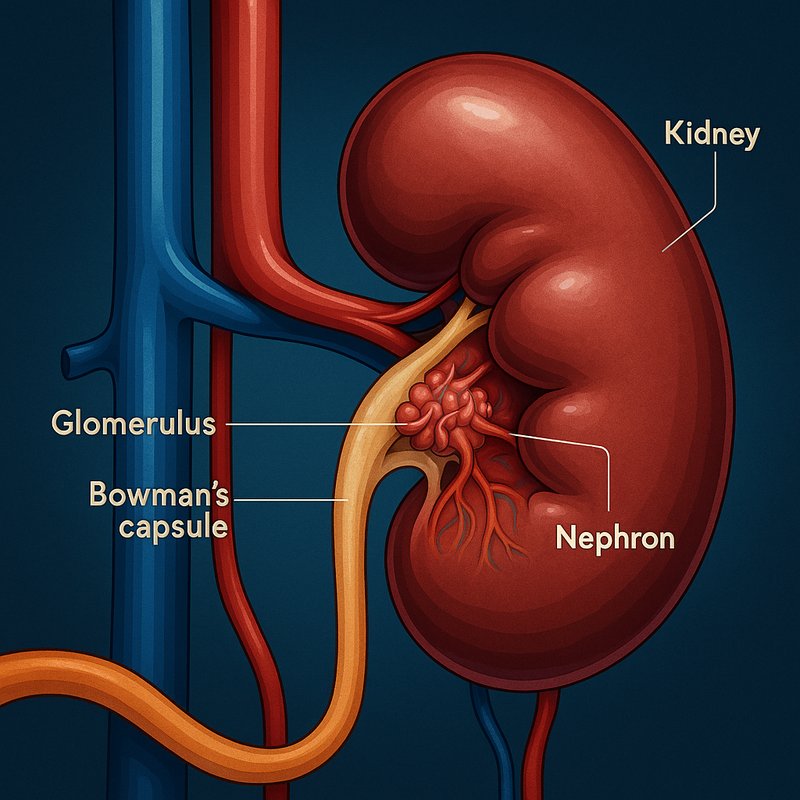
Filtration Power of the Kidneys
Your kidneys filter around 180 liters of fluid every single day — that's your entire blood supply cycling through roughly every four to five minutes. They rely on roughly two million nephrons, each containing a microscopic filtration barrier that blocks large proteins while letting waste pass through. A healthy GFR runs between 80–120 mL/min, but it declines naturally with age. There's much more to uncover about how this system works and what happens when it starts to fail.
Key Takeaways
- Your kidneys filter approximately 180 liters of plasma daily, yet produce only about 1.5 liters of urine through 99.3% tubular reabsorption.
- Kidneys cycle your entire blood supply every 4–5 minutes, processing roughly 1.2 liters of blood per minute continuously.
- Each kidney contains about one million nephrons, tiny filtration units working simultaneously to clean your blood.
- The glomerular filtration barrier blocks red blood cells and large proteins while allowing water, glucose, and small solutes to pass freely.
- A healthy kidney operates at roughly 100 mL/min/1.73 m², filtering about 20% of plasma with each pass.
What Is GFR and Why Is It the Main Measure of Kidney Health?
Kidney health comes down to one key measurement: glomerular filtration rate, or GFR. It tells you how much blood your glomeruli — tiny kidney filters — process each minute.
Specifically, it measures how much plasma your glomerular capillary walls remove from your blood within a given time.
Your doctor calculates your eGFR using blood tests that measure filtration markers like serum creatinine or cystatin C, alongside your age and weight. Creatinine clearance is central to this process, revealing how efficiently your kidneys eliminate waste.
A normal eGFR sits around 100 mL/min/1.73 m², with anything above 60 considered healthy.
Below that threshold, sustained for three or more months, signals chronic kidney disease requiring medical attention. Nearly 90% of people with chronic kidney disease are estimated to be unaware they have it, making routine eGFR testing a critical tool for early detection.
How Much Blood Your Kidneys Actually Filter Every Day
Your kidneys constantly work behind the scenes, filtering roughly 90–120 milliliters of blood every minute. Scale that up, and the daily volume reaches an astonishing 130–173 liters processed every single day. That figure likely surprises most people, since it far exceeds the body's total blood supply.
Here's how it works: your kidneys don't simply filter blood once. They cycle the same blood repeatedly, adjusting plasma composition by removing waste, excess minerals, and fluids while returning what your body still needs. This continuous recycling keeps your bloodstream chemically balanced.
At peak efficiency, healthy kidneys operate at roughly 100 mL/min/1.73 m². Maintaining that rate matters because even a modest, sustained drop signals that waste products are building up faster than your kidneys can clear them. When an eGFR remains below 60 for three consecutive months, it is considered grounds for a chronic kidney disease diagnosis.
The Nephrons, Podocytes, and Filters That Make GFR Possible
Behind those daily filtration numbers sit roughly one million nephrons in each kidney — the actual units doing the work. Nephron density across your renal cortex determines how efficiently your kidneys cleanse blood, and each nephron contains a renal corpuscle, tubule, and capillary network working together.
Inside every renal corpuscle, the glomerulus pushes fluid through a three-layer barrier: endothelial cells, a basement membrane, and podocyte foot processes. Podocyte dynamics matter here because these specialized cells form the innermost filtering layer, and any disruption compromises what passes through. Your filtrate then moves into Bowman's space before traveling through the proximal tubule, loop of Henle, and distal tubule.
Together, these structures sustain the 120 ml/min GFR your kidneys maintain through constant internal feedback. The fenestrated capillaries of the glomerulus allow water, glucose, urea, and ions to pass freely while blocking red blood cells and large proteins under normal conditions.
How Size and Charge Determine What Gets Through the Glomerulus
Once you understand how a nephron's three-layer barrier is assembled, the next question is what actually decides which molecules sail through and which get turned back. Two forces drive glomerular sieving: molecular size and electrical charge.
Size works on a spectrum. Glucose (180 Da) crosses freely, while albumin (69 kDa) barely makes it through. Resistance builds progressively beyond 7,000 Da, and nothing larger than the 25–30 nm slit diaphragm passes the final barrier.
Charge discrimination adds another layer. The glycocalyx, basement membrane, and slit diaphragm all carry negative charges, actively repelling anionic molecules regardless of size. A negatively charged molecule filters far less easily than a same-sized positive one. Together, these two mechanisms create a spectrum-based filter that tightens as both molecular weight and negative charge increase.
The fenestrated glomerular endothelium permits molecules smaller than 70 nm to pass, while the basement membrane imposes an additional restriction of approximately 1 kDa by size and further screens by negative charge.
The Pressure System That Pushes Plasma Into Your Kidneys
Filtration doesn't happen by accident — it's driven by a precise balance of competing pressures that your body constantly fine-tunes. Three forces determine your Net Filtration Pressure: glomerular blood hydrostatic pressure pushes outward at roughly 55 mmHg, while capsular hydrostatic pressure (15 mmHg) and blood colloid osmotic pressure (30 mmHg) push back. That leaves only about 10 mmHg driving filtration forward.
Because that margin is so small, minor shifts in blood osmolarity or capillary pressure dramatically affect filtrate formation. Your kidneys manage this through afferent regulation — dilating or constricting the afferent arteriole to stabilize glomerular pressure. Tubular feedback also signals adjustments when flow rates change. If mean arterial pressure drops below 60 mmHg, these mechanisms can't compensate, and filtration fails. Autoregulation remains effective only within an arterial pressure range of approximately 80–180 mmHg, beyond which the myogenic and tubuloglomerular feedback mechanisms can no longer protect the glomerulus.
Why Your Kidneys Filter 180 Liters But Make 1.5 Liters of Urine
Every day, your kidneys filter roughly 180 liters of plasma — yet you produce only about 1.5 liters of urine. That gap exists because your renal tubules reabsorb nearly 99.3% of filtered fluid back into your bloodstream. This massive recovery effort maintains your fluid balance by selectively retaining water, sodium, potassium, and other essential solutes while discarding waste.
Vasopressin drives much of this process. When your plasma osmolality rises, your kidneys release this hormone, signaling collecting ducts to retain more water. The energy cost of sustaining this system is substantial — your kidneys consume roughly 20% of your cardiac output just to filter and reabsorb at this scale. Your final urine volume reflects what's left after your body reclaims everything it needs. The net filtration pressure driving fluid into the glomerular capsule is only about 10 mm Hg, meaning even small shifts in blood pressure or plasma protein levels can significantly alter how much filtrate your kidneys produce.
The Five GFR Stages and What Each One Means for Kidney Function
When your kidneys lose function, clinicians measure that decline using estimated glomerular filtration rate (eGFR) — a number that reflects how many milliliters of blood your kidneys filter per minute.
Five stages define that decline:
- Stages 1–2 (eGFR 60+): Your kidneys still function adequately, but renal biomarkers may reveal early damage — making lifestyle interventions most effective here.
- Stages 3a–3b (eGFR 30–59): Function drops to mild-to-severe impairment, symptoms emerge, and closer monitoring becomes necessary.
- Stages 4–5 (eGFR below 30): Your kidneys struggle critically, preparation for dialysis or transplant begins, and without intervention, Stage 5 becomes life-threatening.
Understanding where your eGFR falls tells you exactly how hard your kidneys are still working — and what comes next. Alongside eGFR, clinicians also assess urine albumin-to-creatinine ratio to further refine risk and guide management decisions at every stage.
What Your eGFR Number Actually Tells Your Doctor
Your eGFR number gives your doctor a precise snapshot of how well your kidneys are filtering toxins from your blood — measured in milliliters per minute. Doctor interpretation depends on your age, since normal values decline naturally over time — from an average of 116 in your 20s to 75 by age 70.
A reading of 90 or higher indicates healthy function, while anything below 60 signals potential kidney disease. However, a single low result doesn't confirm a diagnosis. Your doctor relies on trend monitoring over at least three months before diagnosing chronic kidney disease.
Your results also include raw creatinine or cystatin C levels, giving your doctor a fuller picture. If your eGFR drops below 60, expect a prompt consultation and possibly additional tests like ultrasound or biopsy. The presence of protein in urine can also indicate kidney damage even when your eGFR appears within a normal range.
How Fast All Your Blood Cycles Through Your Kidneys
Right now, your kidneys are filtering your entire blood supply — roughly 1.2 liters per minute — cycling completely through every four to five minutes.
This blood turnover rate means your kidneys process approximately 180 liters daily. That's extraordinary renal throughput for organs the size of your fist.
Three facts that put this into perspective:
- Filtration fraction: Your kidneys filter only 20% of plasma flowing through them each pass, yet that's enough to clean your entire blood volume repeatedly.
- Healthy benchmark: Normal GFR runs 80–120 mL/min/1.73 m², representing peak filtering efficiency.
- Warning threshold: When GFR drops below 60 mL/min/1.73 m² for three months, chronic kidney disease is officially diagnosed.
Your kidneys never stop working this hard. When doctors need to measure this filtering power, they estimate it through a blood test that measures creatinine, a waste product your kidneys continuously clear, combined with factors like age and sex to calculate your estimated glomerular filtration rate.
Why a Low GFR Is So Often Missed Until Damage Is Done
Despite how hard your kidneys work, most people don't find out they're failing until significant damage is already done — and the data explains exactly why.
Early-stage CKD produces zero symptoms, so you won't feel the warning signs. Meanwhile, clinical inertia delays action: studies show a median 237-day gap between your first abnormal kidney measurement and an actual diagnosis.
Coding gaps make things worse — over 65% of patients meeting laboratory CKD criteria never receive a corresponding diagnostic code in their records.
Doctors also miss subtle signals; a woman with an eGFR placing her in the 10th percentile for her age is often told her numbers look "normal." By the time anyone acts, your treatment window has already narrowed considerably. Research analyzing over 200,000 adults found that 58% of patients with a newly abnormal eGFR never received timely follow-up testing to confirm whether kidney disease was actually present.