Fact Finder - Science and Nature
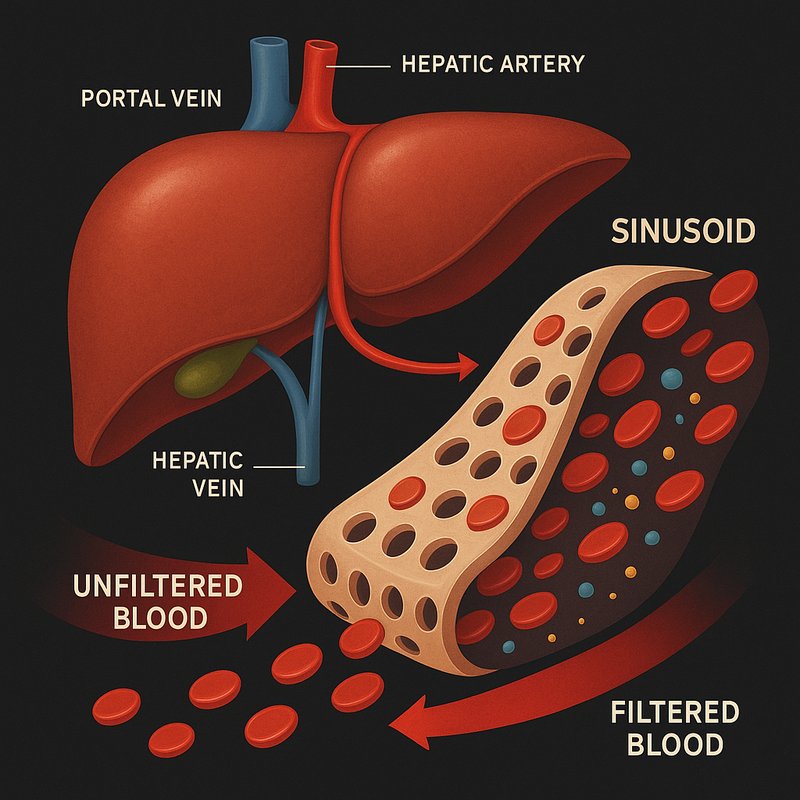
Filtration Power of the Liver
Your liver filters roughly 1.5 liters of blood every minute, processing over 250 gallons daily while holding about a pint in reserve at any moment. It receives blood from two sources — the portal vein and hepatic artery — then moves it through specialized channels called hepatic sinusoids where the actual filtering happens. It's working constantly, even while you sleep. Stick around, because what happens next inside those sinusoids is where things get truly fascinating.
Key Takeaways
- The liver filters approximately 1.5 liters of blood every minute, processing over 250 gallons daily through its hepatic sinusoids.
- It holds roughly one pint of blood at any moment, representing about 13% of the body's total blood supply.
- Blood reaches the liver through two sources: 75% from the portal vein and 25% from the hepatic artery.
- The liver simultaneously filters alcohol, medications, environmental pollutants, and metabolic waste through specialized enzyme pathways continuously.
- Conjugated toxins are exported via bile into the intestines, while water-soluble metabolites exit through urine after renal filtration.
How the Liver Filters 1.5 Liters of Blood Every Minute
The liver quietly takes on one of the body's most demanding jobs — filtering roughly 1.5 liters of blood every single minute. That adds up to over 22 gallons per hour and more than 250 gallons daily. You mightn't feel it happening, but your liver's working constantly beneath the surface.
Blood enters through two pathways, and portal hemodynamics governs how that flow stays balanced and controlled. Once inside, blood moves through the hepatic sinusoid — a specialized channel where filtering actually occurs. Liver cells lining these channels strip out toxins, process nutrients, and neutralize harmful substances before blood continues circulating.
At any moment, your liver holds about a pint of blood — roughly 13% of your body's total supply — giving it that distinctive deep reddish-brown color. By comparison, the kidneys handle their own remarkable feat, receiving 20–25% of cardiac output every minute to carry out the body's precise filtration of plasma through the glomerulus.
The Two-Phase Detox Process Your Liver Runs Nonstop
Behind the liver's constant blood filtration runs a two-phase detox process that never stops. Phase I converts fat-soluble toxins into reactive intermediates through oxidation, reduction, and hydrolysis. Phase II then neutralizes those intermediates through conjugation, attaching molecules like glutathione, sulfate, or glycine to make them water-soluble for safe elimination.
Maintaining phase balance between both stages is critical. If Phase II can't keep up with Phase I output, toxic intermediates accumulate and damage cells. Phase I byproducts that linger without neutralization can cause direct harm to DNA and proteins.
Here's what drives efficient enzyme regulation across both phases:
- Glutathione neutralizes carcinogens, pesticides, and heavy metals
- Sulfation and glucuronidation process hormones and drugs
- Adequate nutrients and energy keep conjugation pathways functioning
Your liver runs this system continuously, processing everything your body encounters.
What Cytochrome P450 Enzymes Actually Do Inside Your Body?
Powering your liver's Phase I detox work are cytochrome P450 enzymes — a family responsible for 80% to 90% of all enzymatic drug metabolism in your body.
Around six key isoforms handle most of this activity, with CYP3A4 processing roughly 30% of clinical drugs and CYP2D6 managing about 20%.
These enzymes don't just break down medications — they also drive steroid synthesis, converting cholesterol into mineralocorticoids, glucocorticoids, and sex hormones.
They're also essential for producing bile acids and fat-soluble vitamins.
Most CYP enzymes operate from your endoplasmic reticulum, targeting foreign substances, while mitochondrial versions focus on internal metabolic functions.
Your genetic makeup directly influences how active these enzymes are, affecting whether drugs work effectively or accumulate to dangerous levels. Over 350 functional polymorphisms have been identified across the human CYP superfamily, meaning individuals can fall into distinct categories such as poor, intermediate, extensive, or ultrarapid metabolizer phenotypes depending on their inherited alleles.
Alcohol, Medications, and Pollutants Your Liver Breaks Down Daily
Every minute, your liver filters approximately 1.5 liters of blood — simultaneously clearing alcohol, medications, environmental pollutants, and metabolic waste without any external help.
Three categories your liver actively processes include:
- Alcohol — Phase I and II enzymes break down alcohol into water-soluble metabolites. Moderate drinking reduces strain on hepatic capacity, with enzyme improvements measurable within weeks.
- Medications — Polypharmacy risks emerge because multiple drugs compete for the same cytochrome P450 pathways, slowing clearance and raising toxicity potential.
- Environmental pollutants — Aflatoxins from contaminated crops and xenobiotics from daily exposure require specialized enzymatic detoxification pathways.
Your liver also neutralizes reactive oxygen species using glutathione and superoxide dismutase — endogenous antioxidant systems requiring no supplementation to function effectively. Chronic liver disease can remain entirely asymptomatic for years, making proactive screening essential for individuals with known risk factors such as excessive alcohol use or a family history of liver disease.
How the Liver Turns Fat-Soluble Toxins Into Excretable Waste
When fat-soluble toxins enter your bloodstream, your liver can't simply flush them out — they resist water-based excretion and would otherwise accumulate in fatty tissues indefinitely. Your liver's Phase I enzymes chemically oxidize and hydrolyze these compounds, converting them into reactive intermediates. Phase II enzymes then bind these intermediates to molecules like glutathione or sulfate, dramatically increasing their water solubility.
Bile carries many conjugated toxins into your intestines, where micelle formation aids their transport through the digestive tract. Some compounds re-enter circulation through enterohepatic recycling, requiring repeated hepatic processing before full elimination. Water-soluble metabolites your kidneys filter exit through urine, while others leave through bile and intestinal excretion. This two-phase biotransformation system prevents toxic bioaccumulation and protects your cells from chemical damage. The liver also removes alcohol from the blood and helps eliminate drug by-products as part of this broader detoxification role.
The Liver's Dual Role in Digestion and Toxin Removal
Your liver operates as both a digestive organ and a detoxification hub simultaneously, making these two functions inseparable in practice.
Bile signaling coordinates fat digestion while amino metabolism converts protein waste into urea for safe excretion. These processes share the same hepatocytes, nutrients, and enzymatic pathways.
Three ways digestion directly supports detoxification:
- Nutrient absorption supplies cofactors that activate Phase I and Phase II detoxification enzymes
- Gut microbiota produce secondary bile acids that support both fat digestion and biotransformation of harmful substances
- Intestinal barrier integrity prevents unwanted toxins from entering circulation, reducing your liver's detoxification workload
When digestion functions properly, your liver detoxifies more efficiently. When detoxification falters, nutrient metabolism suffers. Both systems rise and fall together. The liver receives roughly 75% from the portal vein and 25% from the hepatic artery, meaning the majority of its blood supply arrives directly from the gut and carries absorbed nutrients and toxins together.
Why Your Antioxidant System Is Critical to Liver Health
Constantly under siege from free radicals, your liver depends on a sophisticated two-part antioxidant defense system to survive. This system combines enzymatic defenders—including superoxide dismutases, catalase, and glutathione peroxidases—with non-enzymatic components that neutralize free radicals before they cause damage. Glutathione synthesis plays a central role here, fueling these enzymes while supporting mitochondrial resilience against oxidative assault.
When toxins, alcohol, or poor diet overwhelm these defenses, oxidative stress develops, directly triggering inflammation, fibrosis, and broader liver disease. Your liver's master regulatory switch, the NRF2/ARE pathway, responds by releasing NRF2 from its inhibitor Keap1, sending it into the nucleus to activate cytoprotective and detoxifying genes. Without this system functioning properly, your liver simply can't protect itself. Antioxidants found in foods like citrus fruits, nuts, and leafy greens can help reinforce these natural defenses, reducing the burden of oxidative stress on liver cells.
Foods That Activate Liver Detox Enzymes
Certain foods can kick your liver's detox enzyme systems into high gear, and understanding which ones matter most gives you a real advantage in supporting hepatic function.
Three key dietary categories stand out:
- Cruciferous benefits — Broccoli, kale, and Brussels sprouts contain glucosinolates and sulforaphane, directly boosting detoxification pathways and regulating fatty liver disease.
- Garlic — Organosulfur compounds activate liver enzymes responsible for breaking down environmental toxins, while selenium protects hepatic cells simultaneously.
- Turmeric bioavailability — Curcumin stimulates bile production and enhances enzyme capacity. Preparing golden milk markedly increases curcumin absorption, maximizing its enzyme-activating impact.
Citrus fruits and omega-3-rich fish like salmon further support enzyme function through antioxidant content and anti-inflammatory effects that preserve enzyme-producing hepatocytes. Berries such as blueberries, raspberries, and cranberries deliver antioxidants and polyphenols that protect liver cells and may further reduce the risk of liver disease.