Fact Finder - Science and Nature
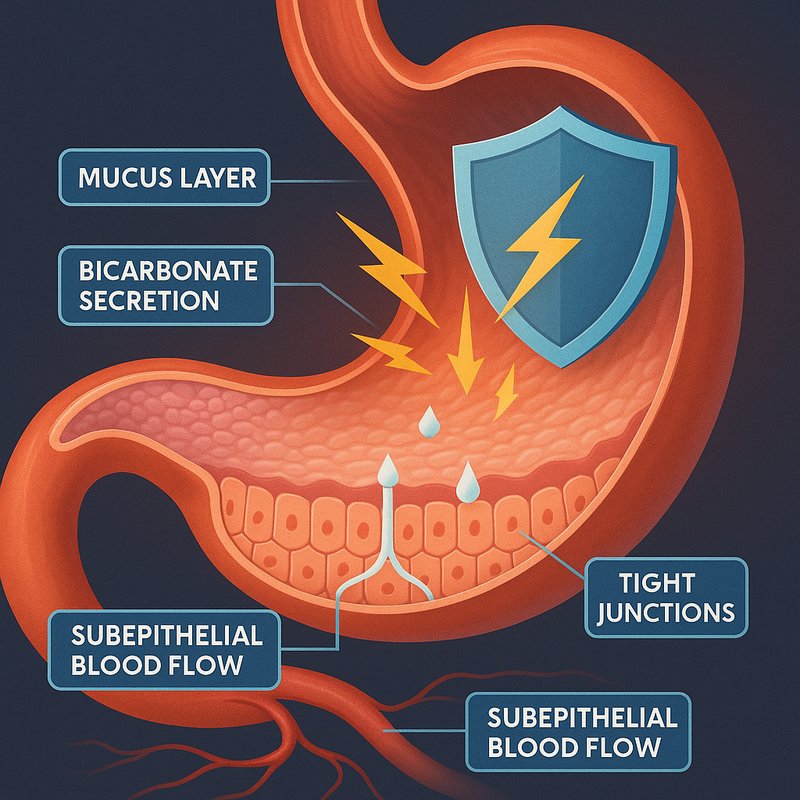
Gastric Mucosa: Stomach Protection
Your stomach lining, called the gastric mucosa, shields delicate tissue from acid strong enough to dissolve metal. It covers over 200 times the surface area of your skin and renews itself constantly through rapid cell turnover. A two-layer mucus system, bicarbonate secretion, and tight cellular junctions work together to prevent self-digestion every single day. There's far more to this remarkable barrier than meets the eye — and it's worth exploring.
Key Takeaways
- The gastric mucosa covers over 200 times the surface area of skin, forming the stomach's primary protective barrier against acid and pepsin.
- A two-layer mucus system traps bicarbonate, creating a pH gradient that neutralizes acid before it reaches the delicate epithelial lining.
- Prostaglandins E2 and I2 enhance mucus and bicarbonate secretion while providing cytoprotection through phospholipids, mucins, and improved mucosal blood flow.
- Tight junctions, hydrophobic membranes, and rapid cell restitution form a second line of defense when the mucus-bicarbonate barrier is compromised.
- NSAIDs, bile salts, and aspirin damage the mucosal barrier by degrading mucus, disrupting microvascular endothelium, and enabling destructive acid back-diffusion.
What Is the Gastric Mucosa and What Does It Protect Against?
The gastric mucosa is the innermost layer of your stomach wall, acting as a primary protective barrier against harmful substances. It lines organs and cavities exposed to external particles throughout your body, covering more than 200 times the surface area of your skin.
Your gastric mucosa serves dual roles in protection and absorption, making it especially significant during digestion. It defends your stomach against its own gastric acid and pepsin, preventing autodigestion and caustic injury. Through mucosal signaling, it coordinates responses to threats, while also managing microbial interactions to maintain a balanced gastric environment.
Cells across its different layers secrete substances that drive these physiological functions, enabling your gastric mucosa to act as your body's most expansive and active protective interface. Its three structural layers — the epithelium, lamina propria, and muscularis mucosae — each contribute distinct roles that collectively sustain mucosal integrity and function.
The Three Layers That Form the Gastric Mucosa
Your gastric mucosa achieves its protective and digestive functions through three distinct layers working in concert.
The innermost epithelial layer lines your stomach with columnar cells, producing alkaline mucus while tight junctions block acid penetration. Stem cells at gastric pit-gland junctions drive rapid mucosal turnover, replacing damaged cells before sustained injury occurs.
Beneath that sits the lamina propria, a loose connective tissue layer housing blood vessels, lymphatics, and immune cells that enable continuous immune surveillance against potential threats. It also surrounds and supports your gastric glands.
The deepest layer, the muscularis mucosae, contains inner circular and outer longitudinal smooth muscle fibers. Its contractions expel gland secretions into your stomach lumen and fold the mucosa into rugae, completing this integrated three-layer defense system. The mucosa as a whole is anchored to the underlying submucosa, a thick and flexible connective tissue layer rich in vasculature and lymphatics that sustains the mucosal layers above.
How Rugae Expand the Gastric Mucosa's Protective Surface
Lining your stomach's inner surface, rugae are prominent ridges composed of flexible mucosal and submucosal tissue that dramatically expand your gastric mucosa's functional area. Through rugae biomechanics, these coiled folds can triple your stomach's surface area, maximizing contact between food and digestive secretions while accommodating varying food volumes without raising internal pressure.
When you eat, mechanoreceptors detect pressure increases, stretching the folds outward as your stomach distends. This expansion supports mucosal perfusion by distributing gastric glands across a wider surface, enhancing secretion of both digestive enzymes and protective mucus.
Simultaneously, epithelial cells seal at tight junctions during stretching, stem cells rapidly replace damaged cells, and bicarbonate-rich mucus maintains a protective coating, collectively shielding your stomach wall from corrosive digestive juices. The submucosal layer, which contains ganglion neurons, adipose tissue, and various vessels and nerves, provides essential structural support to the overlying mucosa during this protective process.
Cell Types in the Gastric Mucosa and What They Do
Rugae give your gastric mucosa the surface area it needs to work effectively, but that surface is only as functional as the specialized cells covering it.
Your stomach's mucosal stem cells continuously replenish six distinct cell types, each following precise secretory pathways to maintain protection and digestion.
Surface mucous cells coat your stomach lining with alkaline mucus and bicarbonate, shielding it from acid. Mucous neck cells reinforce this defense near gland openings.
Parietal cells produce hydrochloric acid and intrinsic factor, while chief cells release pepsinogen and gastric lipase.
Enteroendocrine cells regulate everything through hormones like gastrin, somatostatin, and ghrelin, with ECL cells amplifying acid production via histamine. D-cells secrete somatostatin when lumen acidity reaches a threshold, providing inhibition of gastrin release to prevent runaway acid production.
Together, these cells balance your stomach's corrosive environment with the protection it needs to function safely.
The Five Things That Keep Your Stomach Lining Intact
Five distinct mechanisms work together to keep your stomach lining intact despite the corrosive environment it endures.
First, your mucous layer forms a gel-like barrier that slows acid diffusion toward your epithelial tissue.
Second, bicarbonate secretion creates a pH gradient, neutralizing any H+ ions that penetrate the mucus. Bicarbonate secretion can be triggered by vagal stimulation and fundic distension.
Third, your epithelial cells use tight junctions, hydrophobic membranes, and sulphydryls to block harmful substances from causing damage.
Fourth, adequate blood flow delivers oxygen and nutrients while removing acid that seeps into your mucosa.
Fifth, prostaglandin synthesis reinforces your defenses by enhancing mucus and bicarbonate production, reducing hemorrhagic damage, and supporting tissue repair.
Together, these five layers form an all-encompassing, coordinated system that protects your stomach lining from its own digestive acid.
How the Stomach Lining Protects Itself From Acid
Your stomach lining wages a constant chemical battle against the very acid it produces, relying on five interconnected defense mechanisms to stay intact. Through acid sensing and neural feedback, your body coordinates these defenses dynamically:
- A mucus-bicarbonate barrier traps near-neutral pH directly against epithelial cells
- Tight junctions and phospholipid membranes block acid penetration at the cellular level
- Rapid cell restitution covers damaged areas before deeper injury develops
- Subepithelial blood flow flushes penetrating hydrogen ions and delivers repair nutrients
- Prostaglandins E2 and I2 amplify mucus and bicarbonate secretion while providing direct cytoprotection
Each layer responds to tissue stress signals, triggering accelerated regeneration and vasodilation through nitric oxide pathways.
Your stomach's defense isn't passive — it actively adapts to maintain mucosal integrity continuously. The mucus layer itself is composed of mucins, phospholipids, water, and electrolytes, forming a physical and chemical shield that protects the mucosa from noxious substances and abrasion by stomach contents.
How Gastric Mucosa Mucus Shields Against Acid and Enzymes
Gastric mucus does more than coat your stomach — it operates as a structured, two-layered chemical shield that keeps both hydrochloric acid and proteolytic enzymes from reaching your epithelial tissue.
MUC5AC mucin crosslinking creates a dense inner layer that bacteria and acid can't penetrate, while bicarbonate ions embedded throughout establish a pH gradient from 2 in the lumen to neutral at your epithelial surface.
The outer layer buffers additional enzymatic activity, preventing proteolytic enzymes from auto-digesting your stomach wall.
Surface mucous cells rebuild this inner layer hourly, maintaining continuous protection. Parietal cells in the body and fundic glands secrete intrinsic factor, which is essential for vitamin B12 absorption and healthy red blood cell maturation.
Microbiome interactions within the outer layer also influence mucus stability, as microbial communities affect how effectively the loose layer performs its secondary buffering role against ongoing digestive enzyme activity.
What Damages the Gastric Mucosal Barrier and Triggers Ulcers
Several agents tear through your gastric mucosal barrier through distinct but converging mechanisms. Aspirin induced permeability disrupts your mucus-bicarbonate layer, while bile salts degrade your protective mucus coating. NSAIDs damage your microvascular endothelium within minutes.
Here's how barrier collapse unfolds:
- Microvascular rupture precedes epithelial damage, releasing plasma and erythrocytes
- Blood flow cessation triggers ischemia, which destroys barrier function after 60 minutes
- Free radicals accelerate cascading mucosal destruction
- Epithelial cell death through apoptosis, necrosis, and autophagy collapses structural integrity
- Hydrochloric acid back-diffusion penetrates your lamina propria once barriers fail
When your regenerative capacity can't match injury severity, ulcers form. Persistent exposure to these damaging factors overwhelms your defenses, driving superficial lesions into progressively deeper, harder-to-heal wounds. Reduced expression of survivin, an anti-apoptosis protein that regulates cell survival and proliferation, makes your microvascular endothelial cells significantly more vulnerable to these damaging agents.
What Happens When the Gastric Mucosal Barrier Fails?
Once the gastric mucosal barrier fails, H+ ions diffuse deeper into your tissue faster than bicarbonate can neutralize them. Your tissue buffers become exhausted, triggering acidosis and submucosal damage. Counter-diffusing hydrochloric acid penetrates the lamina propria, causing diffuse injury to deeper gastric structures.
Decreased mucosal blood flow drives ischemic injury by concentrating hydrogen ions while cutting off bicarbonate delivery to neutralize them. Without adequate blood flow, erosions and hemorrhage become nearly inevitable.
Bile-mediated damage compounds the problem when refluxed bile salts disrupt your mucosal barrier. Lipid-soluble bile acids penetrate epithelial cells directly, causing injury from within. Prolonged contact with bile salts and lysolecithin triggers chronic gastritis. If these processes continue unchecked, erosions deepen, bleeding develops, and your gastric structures sustain lasting damage. The question of why the stomach does not digest itself under normal conditions has puzzled scientists since 18th century observations first demonstrated that gastric juice was capable of breaking down meat tissue.
How Your Stomach Lining Heals Itself After Damage
When your stomach lining sustains damage, it doesn't wait passively for recovery — it launches a coordinated repair response driven by growth factor signaling, cellular regeneration, and vascular support.
Key mechanisms include:
- EGF receptors increase 75-fold at ulcer margins, accelerating tissue repair
- Epithelial restitution restores mucosal integrity through cytoplasmic pH homeostasis
- TFF peptides activate EGFR, triggering MAPK and PI3K/Akt signaling pathways
- Nitric oxide enhances blood flow, reduces neutrophil adhesion, and supports wound repair
- Prostaglandins E₂ and I₂ maintain mucosal blood flow while coordinating defense and renewal
Your stomach also simultaneously develops new blood vessels through angiogenesis and vasculogenesis, ensuring damaged tissue receives adequate oxygen and nutrients throughout recovery. Underlying this entire repair process is the mucus-bicarbonate barrier, which serves as the first line of defence against self-digestion by maintaining a protective layer of mucus and bicarbonate directly at the epithelial surface.