Fact Finder - Science and Nature
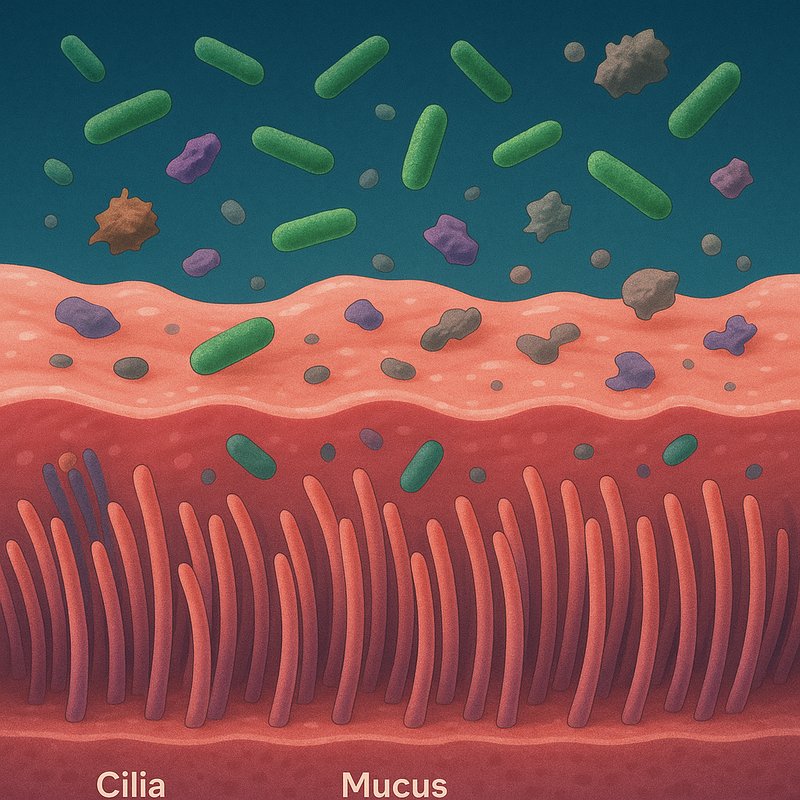
Protective Cilia of the Airway
Your airways are lined with roughly 200 cilia per cell, beating 10–20 times per second in synchronized waves to sweep mucus, bacteria, and debris toward your throat. They're not just mechanical sweepers, though — they can actually taste bacteria and trigger immune responses before infection takes hold. When cilia fail, the consequences range from chronic lung infections to infertility and reversed organ positioning. There's far more to these microscopic structures than you'd expect.
Key Takeaways
- Each airway epithelial cell carries roughly 200 cilia, beating 10–20 times per second to continuously sweep mucus and pathogens toward the throat.
- Airway cilia detect bacterial signals through bitter taste receptors, triggering nitric oxide release that kills bacteria and accelerates ciliary beating simultaneously.
- Cilia operate within a precise two-layer mucus system, requiring a watery inner layer of about 7 micrometers to beat effectively.
- Healthy lungs complete a full mucociliary clearance sweep within 24 hours, moving mucus approximately 1 millimeter per minute.
- When cilia malfunction due to structural defects, as in Primary Ciliary Dyskinesia, patients develop chronic infections, infertility, and reversed organ positioning.
What Are Airway Cilia: and Why Should You Care?
Deep in your airways, millions of microscopic, hair-like projections called cilia line your bronchi and respiratory tract, beating in continuous, coordinated wave patterns to keep your lungs clean and healthy. These specialized organelles extend from ciliated cells throughout your upper and lower airways, playing a critical role in airway development and overall respiratory defense.
You should care because cilia work alongside mucus to form your lungs' primary innate defense system. Proper mucosal hydration maintains the periciliary liquid layer, enabling rapid ciliary beating that traps and expels dust, bacteria, viruses, and pollutants. Importantly, cilia are absent from your alveoli, making their protective role in the upper airways essential for preventing harmful contaminants from reaching those vulnerable gas-exchange zones. Scattered among the cilia, goblet cells secrete mucus that traps microorganisms before they can travel deeper into the respiratory system.
The 9+2 Axoneme: What Gives Cilia Their Beating Power
What makes cilia beat with such remarkable coordination? It's the 9+2 axoneme — nine doublet microtubules surrounding two central singlets. This architecture, conserved from algae to humans, forms the structural backbone of every motile cilium you have lining your airways.
Understanding axonemal mechanics helps explain how movement actually happens. Dynein motor proteins generate sliding forces between adjacent doublets, with inner dynein arms shaping waveform size while outer arms double beat frequency. Nexin links convert that sliding into coordinated bending rather than chaotic separation.
Dynein regulation keeps everything controlled. Kinases like PKA phosphorylate axonemal proteins, modulating motor activity and beat frequency. The central pair complex communicates with radial spokes to fine-tune dynein-driven sliding, ensuring your cilia sweep mucus and debris upward with consistent, purposeful rhythm. Defects in this architecture are directly tied to Primary Ciliary Dyskinesia, a condition that impairs mucociliary clearance and can lead to chronic respiratory infections.
The Two-Layer Mucus System Airway Cilia Depend On
Beneath the beating cilia of your airways lies a precisely engineered two-layer system that makes mucociliary clearance possible.
The inner periciliary dynamics involve a thin, watery sol layer roughly 7 μm deep, allowing cilia to beat freely at 10–20 Hz while staying in contact with the overlying mucus gel. That gel layer, reaching 50 μm thick in large airways, traps pathogens, particles, and toxins before cilia propel everything toward your mouth.
Mucin biochemistry drives the gel's function. MUC5B forms long polymer chains cross-linked by calcium, creating viscoelastic properties essential for effective transport. Glycan side chains bind water at hundreds of times their molecular weight.
Submucosal glands, goblet cells, and Clara cells collectively maintain both layers, keeping your airways continuously protected and clear. Alongside mucins, the airway surface liquid carries protective macromolecules with anti-microbial, anti-protease, and anti-oxidant activity that collectively strengthen the defensive capacity of the mucus layer.
How Airway Cilia Clear Your Lungs Daily
Every breath you take sets off a remarkable coordinated sweep through your airways. Your cilia beat in synchronized metachronal waves, propelling trapped pathogens and particles from peripheral airways toward your throat. Mucus moves roughly 1 mm per minute, traveling from smaller bronchi through larger airways until it reaches the trachea and gets swallowed or expelled.
Daily clearance depends entirely on proper airway hydration. Your body produces 20–30 ml of secretions daily, and ion channels CFTR and ENaC regulate the moisture levels keeping that mucus moving efficiently. When production exceeds this range, your cough reflex activates as backup.
The result is impressive: your healthy lungs complete a full sweep in under 24 hours, continuously protecting delicate lung tissue from inhaled particles and pathogens. Each epithelial cell bears approximately 200 cilia that beat 10–20 times per second, driving this relentless protective process around the clock.
How Airway Cilia Can Actually Taste Bacteria
Your airway cilia don't just move—they taste. Embedded directly on your motile cilia are bitter taste receptors called T2Rs, the same receptor type found on your tongue. This bitter sensing cilia system performs microbial chemoception by detecting bacterial quorum-sensing molecules called acyl-homoserine lactones before bacteria reach dangerous densities.
When T2R38 receptors detect these compounds, they trigger an immediate calcium release, which boosts nitric oxide production. That nitric oxide then diffuses directly into bacterial cells, destroying their DNA while simultaneously accelerating your cilia's beating frequency to physically sweep pathogens out.
Your cilia also signal neighboring cells to release antimicrobial peptides, creating a dual-elimination response—all without involving your nervous system. Notably, when cilia are lost due to smoking or disease, the airway's ability to detect and respond to harmful inhaled chemicals becomes significantly compromised.
The Real-World Consequences of Ciliary Dysfunction
When your cilia's bitter taste receptors fail—or when the cilia themselves are structurally defective—the consequences cascade across nearly every organ system that depends on ciliary motion.
Mucus accumulates in your lungs, enabling bacterial colonization, chronic infection, and eventual bronchiectasis.
Your sinuses and ears suffer recurrent infections, sometimes causing permanent hearing loss.
Fertility impacts are direct: men produce immotile sperm, while women face increased ectopic pregnancy risk from impaired oviduct cilia.
About 50% of patients develop reversed organ positioning.
Surgical outcomes worsen considerably—infants with abnormal ciliary motion require extended ventilation and more respiratory medications after cardiac surgery.
Low nasal nitric oxide levels even predict poor post-surgical cardiac function.
Across all systems, structural damage accumulates, making early screening and long-term management essential. Because the condition stems from pathogenic gene variants, it cannot be prevented, making genetic counseling an important resource for families with a history of the disorder.
Cystic Fibrosis, PCD, and What Happens When Cilia Fail
Though they share a common outcome—progressive lung disease beginning in early childhood—cystic fibrosis and primary ciliary dyskinesia arrive there through entirely different mechanisms. CF disrupts salt transport in airways, while PCD stems from congenital defects in ciliary structure or function. Despite these distinctions, both conditions demand early intervention through neonatal screening and genetic counseling to prevent irreversible damage.
What's striking is how severely PCD challenges the assumption that it's the milder disease. Children with PCD involving inner dynein arm and microtubular defects actually showed lower lung function than CF minimal-function groups by age 10, with the gap widening further by age 14. When your cilia fail—regardless of why—the consequences are anything but minor. Unlike CF, which benefits from established therapeutic approaches, PCD treatment remains largely dependent on consensus guidelines and extrapolation from CF evidence due to limited disease-specific research.
How Cilia Do More Than Clear Mucus: Immunity, Repair, and Sensing
Cilia do far more than sweep mucus out of your airways—they're active participants in your immune defense, sensing threats and coordinating responses before pathogens ever reach deeper tissue. They express bitter taste receptors (T2Rs) that detect bacterial signals and trigger immediate innate immune responses.
Your epithelial cells amplify this by releasing cytokines like IL-15, TSLP, and type I interferons, driving immune signaling that activates dendritic cells and promotes protective Th1 responses in lymph nodes.
Cilia also contribute to epithelial regeneration after infection damages tissue. Epithelial-derived growth factors coordinate with cytokine networks to restore barrier integrity. When cilia malfunction, this repair capacity weakens, prolonging recovery and increasing vulnerability to secondary infections. During viral infection, epithelial cells release chemokines, cytokines, alarmins, and matrikines that amplify pre-existing airway inflammation and contribute to acute exacerbation formation. Your cilia aren't passive tubes—they're dynamic sensors woven into your respiratory defense system.