Fact Finder - Science and Nature
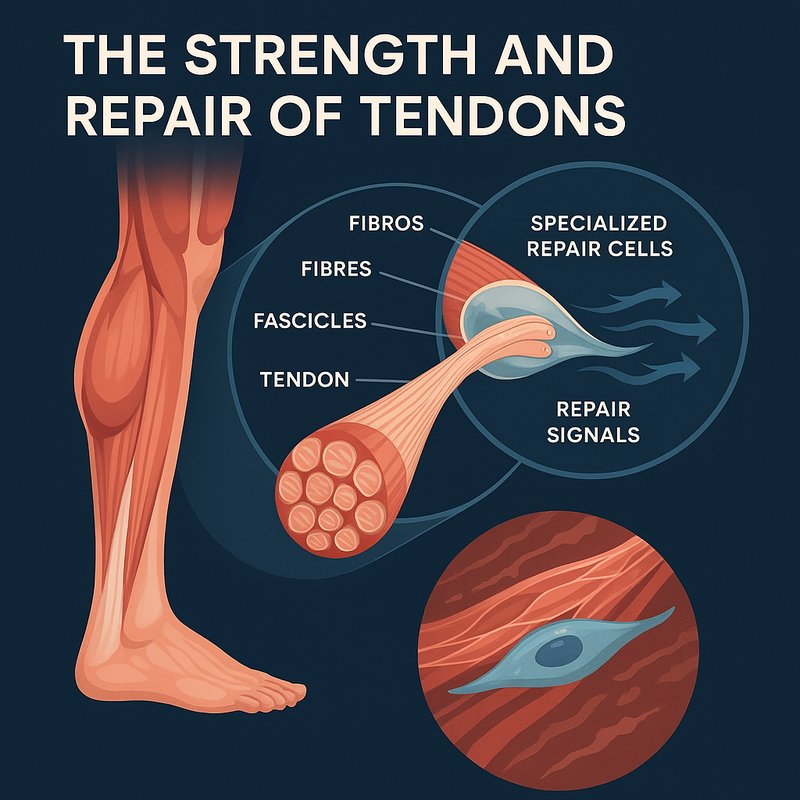
Strength and Repair of Tendons
Your tendons are stronger than most people realize — the Achilles alone handles six to eight times your body weight during maximal sprints. Type I collagen forms their primary load-bearing structure, while specialized cells constantly detect mechanical stress and trigger repair signals. Tendons can increase stiffness by over 57% with proper high-intensity loading, and genetic variants even influence how stiff yours naturally are. There's far more happening inside these structures than you'd expect.
Key Takeaways
- Tendons are organized hierarchically—from molecules to fascicles—dramatically amplifying load-bearing capacity beyond what individual collagen fibers could achieve alone.
- The Achilles tendon endures forces six to eight times body weight during maximal sprinting, showcasing extraordinary tensile strength.
- After injury, tendons first deposit weaker type III collagen before gradually replacing it with stronger type I collagen during maturation.
- High-intensity loading at approximately 80% of maximum effort produced a 57.7% increase in tendon stiffness over just 12 weeks.
- Repair enzymes reactivate every six hours, making spaced high-effort training sessions more effective than frequent low-load approaches.
What Gives Tendons Their Remarkable Strength and Stiffness?
Tendons derive their remarkable strength and stiffness primarily from Type I collagen, which makes up 65–85% of their dry weight and serves as the main load-carrying component.
Its collagen architecture follows a precise hierarchical progression—molecules bundle into fibrils, fibers, fascicles, and finally the complete tendon unit. This layered organization amplifies load-bearing capacity at every level.
Fibers align longitudinally along the tendon axis while also crossing in spiral arrangements, creating a crimp pattern that stores elastic energy and resists tensile forces. Crosslink density between tropocollagen molecules converts soluble proteins into insoluble, high-strength collagen aggregates.
Supporting components like elastin, proteoglycans, and glycoproteins contribute resilience and mechanical stability. Together, these structural features give you a tissue engineered to withstand extraordinary mechanical demands. The entire tendon unit is encased in a surrounding sheath called the epitenon, which reduces friction during movement.
How Do Tendons Detect and Respond to Mechanical Load?
Built into tendon's structural hierarchy is a living sensory system that doesn't just passively bear load—it actively reads mechanical signals and responds. Your tenocytes detect force through mechanosensitive receptors, converting external loads into precise biochemical instructions that regulate cell behavior and matrix remodeling. This cytoskeletal signaling creates bidirectional communication between the cell's internal framework and the surrounding extracellular matrix, maintaining dynamic homeostasis and enabling adaptation to shifting mechanical demands.
When you apply appropriate tensile loads through running or resistance training, this system triggers anabolic gene expression—upregulating scleraxis, type-I collagen, and tenomodulin. Conversely, when loading drops, these pathways quiet down, reducing collagen production and compromising tendon stiffness. The type of load also matters: tension drives tendon-specific differentiation, while sustained compression pushes cells toward cartilage-like tissue formation. High levels of prostaglandin E2 can signal tendon progenitor cells to differentiate into adipocytes and chondrocytes, implicating aberrant PGE2 signaling in the fatty infiltration, fibrosis, and calcification observed in degenerating tendons.
What Training Intensity Do Your Tendons Actually Need?
Unlike passive structures that simply respond to whatever load you throw at them, tendons require a minimum intensity threshold before they'll adapt structurally. Research confirms that training below roughly 40% of your one-rep max fails to trigger meaningful structural changes, even if maximal tendon force increases slightly.
High intensity loading—around 80% of 1RM—produced a 57.7% increase in tendon stiffness over 12 weeks, while low-intensity protocols produced none. Your load threshold matters more than volume or frequency.
Isometric duration also plays a significant role. Holds lasting 30–45 seconds at approximately 70% of maximum voluntary contraction optimize tendon nourishment and structural remodeling. For recovery scheduling, tendon repair enzymes reactivate every six hours, making spaced, high-effort sessions more effective than frequent low-load training. A large-scale systematic review and meta-analysis of over 3,900 participants further supports this, finding that less-than-daily training frequency is more likely to enhance tendinopathy recovery than more frequent regimens.
How Do Your Cells Rebuild and Stiffen Tendon Fibers?
When your tendon sustains damage, a tightly coordinated molecular repair sequence activates almost immediately. Growth factor signaling drives the entire process, with TGF-β, IGF-1, and bFGF directing fibroblasts to rebuild your extracellular matrix.
Your cells follow three distinct rebuilding stages:
- Early collagen deposition – Fibroblasts rapidly produce type III collagen, establishing a temporary scaffold
- Cellular alignment – Tenocytes sense mechanical stress and reorient fibers along load-bearing pathways
- Matrix maturation – MMPs degrade disorganized collagen while type I collagen gradually replaces type III, restoring tensile strength
bFGF accelerates this shift by activating NF-κB gene expression, stimulating DNA synthesis, and promoting organized collagen arrangement. Your tendon's final stiffness depends heavily on how completely this type III-to-type I collagen shift occurs. Tendons are particularly vulnerable to slow, poor-quality healing because of their inherently low vascularity and reduced metabolic activity.
Why Are Some People's Tendons Naturally Stiffer?
Genetics plays a central role in why your tendons may feel naturally more rigid or flexible than someone else's. Your genetic predisposition shapes how your body produces and organizes collagen, the primary structural component of tendons. Variations in genes like COL5A1 and COL1A1 directly influence collagen fibril width, quality, and overall matrix organization. For example, carrying the TT genotype at COL5A1's rs12722 increases your risk of Achilles tendon pathology, while the CC genotype offers measurable protection.
Collagen aging compounds these genetic differences. As you get older, your total collagen content decreases, yet the remaining collagen becomes stiffer due to increased cross-linking and fiber organization. Combined with your unique genetic profile, these age-related shifts determine your tendon's natural stiffness level. Notably, genes like COL11A1 have also been implicated in tendon vulnerability, with a specific TCT(AGGG) haplotype found in 25% of Achilles tendinopathy patients compared to just 9.1% of controls.
Why Tendon Stiffness Matters More During Explosive Movements
Explosive movements demand far more from your tendons than slow, controlled ones.
During high-velocity actions, your tendons face rapid force spikes requiring immediate impact mitigation and efficient elastic recoil. Stiff tendons handle this better by transmitting force quickly without losing energy.
Here's why stiffness becomes critical during explosive efforts:
- Peak tendon strain increases markedly at faster movement speeds, requiring structural integrity under heavier elastic loading.
- Rate of force development rises sharply, meaning your tendons must absorb and release energy within milliseconds.
- Tendon hysteresis decreases after explosive training, reducing energy loss during repeated high-velocity efforts.
Slow exercises simply don't replicate these demands.
Your tendons adapt specifically to the speed and intensity they're trained under. During sprint contacts at maximum velocity, your Achilles tendon alone can handle six to eight times body weight.
Can Children's Tendons Get Stiffer From Resistance Training?
These stiffness gains come from changes in tendon material properties, not hypertrophy, which is relevant when growth plate considerations shape your training decisions. Resistance training also increased resting fascicle length by 2.2 mm and reduced electromechanical delay by 13%, confirming that children's tendons respond meaningfully to progressive mechanical loading. In children with cerebral palsy, compliant tendons absorb a disproportionate amount of joint rotation stretch, reducing the mechanical stimulus that reaches muscle fascicles.
How Do You Know Your Tendons Are Actually Adapting?
Measuring tendon adaptation requires objective tools, not just how your tendon feels after training. Ultrasound monitoring tracks real biomechanical markers that confirm whether your tendon is genuinely responding to load.
Three measurable indicators confirm tendon adaptation:
- Stiffness changes — Ultrasound combined with dynamometry quantifies stiffness during maximal isometric contractions, reflecting current muscle-tendon adaptation levels.
- Cross-sectional area (CSA) — CSA correlates markedly with activity level, providing an objective loading response indicator.
- Tendon length shifts — Longitudinal dimension changes tracked via B-mode ultrasound signal structural adaptation under mechanical loading.
Without these measurements, you're guessing. Standardized ultrasound protocols minimize positional and observer errors, ensuring your adaptation data stays accurate and actionable. Research tracking elite jumpers over four years found that muscle and tendon adaptations do not always progress in sync, with tendons showing greater fluctuations in stiffness and strain compared to muscle strength gains.