Fact Finder - Science and Nature
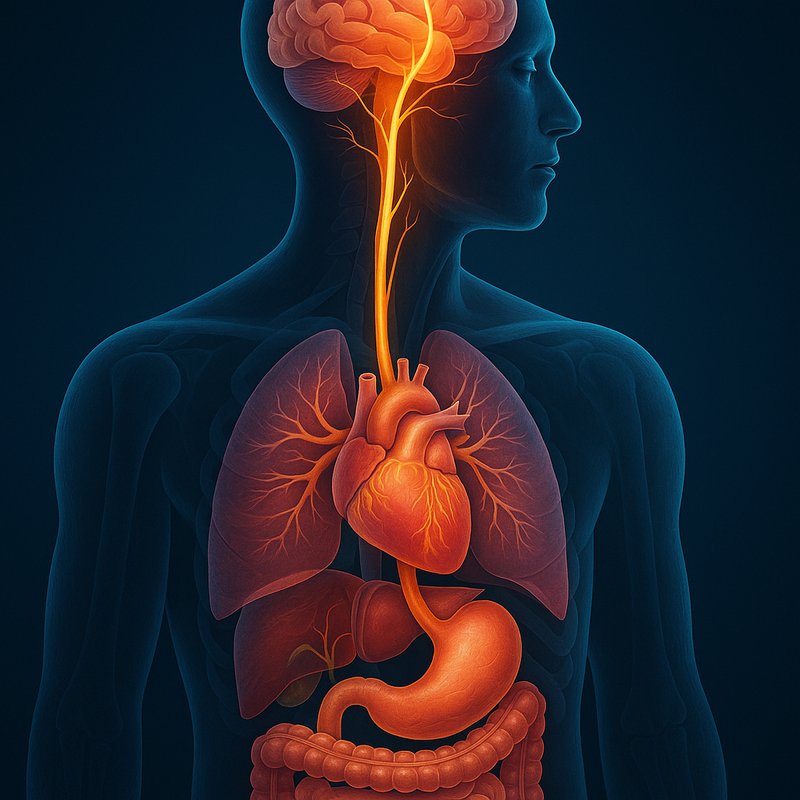
Vital Function of the Vagus Nerve
Your vagus nerve is the longest cranial nerve in your body, stretching from your brainstem all the way down to your colon. It's quietly running the show every second of your life, controlling your heart rate, digestion, breathing, and even your immune response. Its sensory fibers make up 80–90% of its total fibers, meaning it's mostly listening, not talking. There's far more to this remarkable nerve than you'd expect.
Key Takeaways
- The vagus nerve is the body's longest autonomic nerve, connecting the brain to the heart, lungs, gut, and beyond.
- It acts as a natural heart rate regulator, slowing the intrinsic rate from ~100 bpm down to a healthy 60–80 bpm.
- Roughly 80–90% of vagus nerve fibers are sensory, transmitting visceral information from organs back to the brain.
- It controls digestion by signaling acid secretion, enzyme release, and peristalsis while also detecting nutrient composition and microbiome signals.
- The vagus nerve activates an inflammatory reflex that suppresses harmful cytokine production, directly linking it to immune system regulation.
What Exactly Is the Vagus Nerve?
The vagus nerve is the 10th cranial nerve (CN X) and the longest nerve in your autonomic nervous system. Its name derives from the Latin word for "wandering," which perfectly describes its extensive path through your body.
Originating in your medulla oblongata, it exits your skull through the jugular foramen, traveling through your neck, chest, and abdomen, reaching as far as your colon.
It's a functionally diverse nerve, containing both motor and sensory fibers — with sensory fibers comprising 80-90% of its composition.
These sensory fibers handle visceral perception, relaying critical information about your organ states to your central nervous system.
Meanwhile, vagal modulation controls essential involuntary functions, including your heart rate, breathing, digestion, and inflammation response. Within the nerve itself, distinct nuclei serve specific roles — for example, the nucleus ambiguus provides the motor fibers responsible for swallowing and phonation, while the dorsal motor nucleus governs autonomic output to your heart, lungs, and gut.
Where Does the Vagus Nerve Actually Travel?
Starting in your brainstem's medulla oblongata, the vagus nerve winds its way through nearly your entire body — from your skull down to your colon. It exits your skull through the jugular foramen alongside cranial nerves IX and XI, then follows a cervical pathway down through your neck inside the carotid sheath.
Once it reaches your chest, thoracic branching causes the left and right vagus nerves to diverge. Your right vagus travels anterior to the subclavian artery, while your left passes between the carotid and subclavian arteries over the aortic arch. Both eventually wrap around your esophagus, forming a nerve plexus.
From there, the vagus passes through your diaphragm's esophageal hiatus, branching into your stomach, pancreas, kidneys, and intestines. Notably, the left recurrent laryngeal nerve hooks under the aortic arch, making it especially vulnerable to irritation from nearby thoracic structures.
How Does the Vagus Nerve Control Your Heart Rate?
Once the vagus nerve reaches your chest, it doesn't just pass through — it takes direct control of your heart's rhythm. Without it, your heart would beat around 100 times per minute. The vagus nerve's constant signaling, called the "vagal brake," pulls that rate down to a healthier 60–80 beats per minute.
What makes this system remarkable is its beat-to-beat control. Your vagus nerve fires once per heartbeat, syncing precisely with your pulse. Vagal timing matters enormously here — bursts arriving earlier in the cardiac cycle lower your heart rate more effectively.
This split-second precision also drives heart rate variability, the natural fluctuation between beats that signals a well-balanced autonomic nervous system. Disrupting this timing can trigger unstable, alternating heart rhythms. Clinicians can deliberately activate this nerve-heart pathway through physical actions like breath-holding or face immersion in ice water, techniques known as vagal maneuvers, which are used as a first-line treatment to slow excessively fast heart rhythms.
How Does the Vagus Nerve Regulate Digestion and Gut Health?
When food hits your stomach, the vagus nerve takes charge of nearly every step that follows. It signals acid secretion, controls muscular contractions, and monitors nutrient composition through specialized receptors along your gut lining. It also responds to microbiome signaling, processing chemical messages from gut bacteria that influence digestion and immune responses.
The vagus nerve manages several critical digestive functions:
- Acid and enzyme release – triggers gastric acid and digestive enzymes needed for proper breakdown
- Peristalsis control – coordinates wave-like muscle contractions that move food forward
- Nutrient sensing – detects fat, protein, and sugar composition to regulate absorption
- Appetite regulation – relays leptin and cholecystokinin signals to suppress hunger
When vagal function weakens, visceral inflammation increases and gastroparesis can develop, severely disrupting normal digestive efficiency. Gastroparesis is commonly caused by damage to the vagus nerve from conditions such as diabetes, viral infection, or abdominal surgery.
How Does It Regulate Your Breathing?
Every breath you take involves the vagus nerve, which extends from your brain stem to directly innervate your lungs through efferent fibers that control airway size and volume.
It directly controls exhalation while becoming attenuated during inhalation, meaning exhalation emphasis is your most powerful tool for vagal activation.
When you slow your breathing and extend your exhales, you signal relaxation to your vagus nerve, shifting your autonomic system away from fight-or-flight toward rest-and-digest mode.
Diaphragmatic pacing amplifies this effect by using intentional breath-work to stimulate vagal afferent fibers in your airways, which transmit feedback signals directly to your central nervous system.
Just a few minutes of deep, extended exhalation breathing can maintain vagal activity and restore autonomic balance. A practical technique is to breathe in through your nose for a count of six and exhale through your mouth for a count of eight, allowing your belly to expand and contract with each breath cycle.
How Does Your Brain Receive and Process Vagus Nerve Signals?
These overlapping pathways let your vagus nerve influence cognition, mood, and neural plasticity through a coordinated, intensity-dependent cascade of electrochemical signals. Factors such as stimulation parameters, administration site, and timing relative to learning tasks critically determine the extent of memory enhancement outcomes.
How the Vagus Nerve Keeps Your Organ Systems in Balance
Your vagus nerve acts as a master regulator, quietly coordinating your cardiovascular, digestive, immune, and mental health systems through parasympathetic nervous system control. It slows your heart rate, supports peristalsis, triggers digestive enzyme release, and activates the inflammatory reflex to suppress harmful cytokine production.
When your body faces illness or injury, your vagus nerve balances immune responses, preventing excessive inflammation that drives autoimmune disorders and neurodegenerative conditions.
Your vagal tone directly shapes stress recovery—high tone means faster return to baseline after stressful events, better mood stability, and reduced depression risk. Low vagal tone disrupts this balance, creating sympathetic dominance that manifests as anxiety, fatigue, and digestive dysfunction.
Maintaining strong vagal tone keeps all these interconnected systems functioning efficiently, supporting your overall health and resilience. The vagus nerve originates in the medulla oblongata of the brainstem and extends its branches throughout the neck, chest, and abdomen to reach the heart, lungs, liver, stomach, and intestines.